Insomnia
Insomnia is a sleep-wake disorder characterised by persistent difficulty with sleep initiation, maintenance, consolidati... MRCP, MRCPsych exam preparation.
What matters first
Insomnia is a sleep-wake disorder characterised by persistent difficulty with sleep initiation, maintenance, consolidati... MRCP, MRCPsych exam preparation.
Suicidal Ideation (Insomnia is a Risk Factor for Suicide)
7 Jan 2026
Generated educational material; verify before clinical use.
Visible references section
See the concept before reading it
Study the key anatomy, imaging, and decision pathways as full teaching plates.
Clinical board
A visual summary of the highest-yield teaching signals on this page.
Urgent signals
Safety-critical features pulled from the topic metadata.
- Suicidal Ideation (Insomnia is a Risk Factor for Suicide)
- Substance Misuse (Alcohol, Sedatives, Stimulants)
- Underlying Obstructive Sleep Apnoea (OSA) - Snoring, Apnoeas, Excessive Daytime Sleepiness
- Symptoms Suggesting Narcolepsy (Cataplexy, Sleep Paralysis, Hypnagogic Hallucinations)
Exam focus
Current exam surfaces linked to this topic.
- MRCP
- MRCPsych
- MRCGP
Linked comparisons
Differentials and adjacent topics worth opening next.
- Obstructive Sleep Apnoea
- Restless Legs Syndrome
Content status and exam context
This page is AI-generated educational content. It may contain errors or omissions and is not a substitute for current guidelines, local protocols, senior clinical judgement, or professional medical advice.
MedVellum does not claim an individual clinician reviewer, board certification, or professional credential for this page unless a future version names a real, verifiable reviewer.
Clinical explanation and evidence
Insomnia
1. Clinical Overview
Summary
Insomnia is a sleep-wake disorder characterised by persistent difficulty with sleep initiation, maintenance, consolidation, or quality despite adequate opportunity and circumstances for sleep, resulting in clinically significant daytime impairment. [1] Chronic Insomnia Disorder (CID) is defined by the International Classification of Sleep Disorders, 3rd Edition (ICSD-3) and DSM-5 as sleep difficulties occurring ≥3 nights per week for ≥3 months. [2,3] It is distinguished from short-term or acute insomnia, which lasts less than 3 months and is often precipitated by identifiable stressors.
Insomnia is the most common sleep disorder, affecting approximately 10-15% of adults with chronic insomnia and up to 30-40% reporting occasional insomnia symptoms. [4] The disorder has a female preponderance (approximately 1.4:1 female-to-male ratio) and increases with age, particularly after menopause. [5] It is frequently comorbid with psychiatric conditions (depression, anxiety disorders), medical conditions (chronic pain, cardiovascular disease, COPD, GORD), and other sleep disorders (obstructive sleep apnoea, restless legs syndrome). [6]
The pathophysiology is conceptualised through the Spielman 3P Model (Predisposing, Precipitating, Perpetuating factors) and the Hyperarousal Model, which posits that chronic insomnia involves sustained physiological and cognitive hyperarousal. [7] Sleep architecture studies demonstrate reduced total sleep time, prolonged sleep onset latency, increased wake after sleep onset, and alterations in sleep stages.
First-line treatment is Cognitive Behavioural Therapy for Insomnia (CBT-I), which has the strongest evidence base for efficacy and durability. [8,9] CBT-I typically involves 4-8 sessions and includes sleep restriction therapy, stimulus control, cognitive therapy, relaxation training, and sleep hygiene education. Digital CBT-I platforms (e.g., Sleepio) have demonstrated comparable efficacy to face-to-face delivery. [10]
Pharmacotherapy should be reserved for short-term use (2-4 weeks maximum) when CBT-I is unavailable, ineffective, or as adjunctive therapy during acute exacerbations. [11] Options include Z-drugs (zopiclone, zolpidem), short-acting benzodiazepines (temazepam), and melatonin (prolonged-release formulation for patients ≥55 years). Long-term hypnotic use is discouraged due to risks of tolerance, dependence, next-day sedation, falls (especially in elderly), and cognitive impairment. [12]
Prognosis is favourable with appropriate treatment. CBT-I achieves remission or significant improvement in 70-80% of patients, with effects maintained at 1-2 year follow-up. [13] However, insomnia often follows a chronic, waxing-and-waning course, and addressing comorbid conditions is essential for optimal outcomes.
Clinical Pearls
CBT-I is First-Line, Not Medication: Cognitive Behavioural Therapy for Insomnia has superior long-term efficacy compared to pharmacotherapy and should be the primary treatment for chronic insomnia. [8,9]
"3-3 Rule" for Chronic Insomnia: Symptoms must occur ≥3 nights per week for ≥3 months to meet diagnostic criteria for Chronic Insomnia Disorder. [2,3]
Avoid Long-Term Hypnotic Prescribing: Z-drugs and benzodiazepines are for short-term use only (2-4 weeks maximum). Prolonged use leads to tolerance, dependence, rebound insomnia, falls, and cognitive impairment, particularly in elderly patients. [12]
Always Screen for Comorbidities: Depression, anxiety, OSA, restless legs syndrome, chronic pain, and substance use are common comorbidities that must be identified and addressed. [6]
Daytime Impairment is Essential for Diagnosis: The presence of nocturnal sleep difficulty alone is insufficient; clinically significant daytime consequences (fatigue, cognitive impairment, mood disturbance) are required. [2,3]
Sleep Diary is the Gold Standard Assessment Tool: A 2-week prospective sleep diary provides objective data on sleep patterns, variability, and sleep-wake schedule, and is essential for diagnosis and monitoring treatment response. [14]
2. Epidemiology
Prevalence and Incidence
- Chronic Insomnia: Affects 10-15% of the adult population, defined as symptoms ≥3 nights per week for ≥3 months. [4]
- Occasional Insomnia Symptoms: Up to 30-40% of adults report transient or occasional sleep difficulties. [4]
- Short-Term Insomnia: Approximately 15-20% of adults experience acute insomnia (lasting less than 3 months), often triggered by stressful life events. [5]
- Increasing Incidence: Prevalence has increased over recent decades, potentially related to increased screen time, shift work, and societal stressors. [15]
Demographics
| Demographic Factor | Epidemiological Pattern |
|---|---|
| Sex | Female > Male (approximately 1.4:1 ratio). Risk increases in women after menopause, likely related to hormonal changes and vasomotor symptoms. [5] |
| Age | Prevalence increases with age. Chronic insomnia affects 12-20% of adults ≥65 years, compared to 8-10% of younger adults. [4,16] |
| Socioeconomic Status | Higher prevalence in lower socioeconomic groups, associated with increased stress, shift work, and reduced access to healthcare. [5] |
| Occupation | Shift workers, healthcare professionals, and those in high-stress occupations have elevated risk. [17] |
| Ethnicity | Some evidence suggests higher prevalence in certain ethnic groups (e.g., African Americans), though findings are inconsistent and may reflect socioeconomic confounding. [5] |
Comorbidities and Associations
Insomnia is frequently comorbid with psychiatric, medical, and other sleep disorders. The relationship is often bidirectional.
| Comorbid Condition | Prevalence / Association | Notes |
|---|---|---|
| Major Depressive Disorder | 50-90% of patients with depression have insomnia. [6] Conversely, insomnia is a risk factor for developing depression (RR ~2.0). [18] | Bidirectional relationship: Insomnia is both a symptom of depression AND an independent risk factor for incident depression. Early morning awakening is classically associated with depression. |
| Generalized Anxiety Disorder (GAD) | 50-70% of patients with GAD report insomnia, particularly sleep onset insomnia due to racing thoughts and rumination. [6] | Anxiety-related insomnia typically involves difficulty initiating sleep rather than early morning awakening. |
| Chronic Pain Syndromes | 50-80% of patients with chronic pain (fibromyalgia, arthritis, neuropathic pain) report insomnia. [6] | Pain disrupts sleep, and sleep deprivation lowers pain threshold, creating a vicious cycle. |
| Obstructive Sleep Apnoea (OSA) | 30-50% of patients with OSA report insomnia symptoms (comorbid insomnia and sleep apnoea, "COMISA"). [19] | OSA must be excluded if snoring, witnessed apnoeas, or excessive daytime sleepiness are present. Treating OSA alone may not resolve insomnia; both conditions require treatment. |
| Restless Legs Syndrome (RLS) | 20-30% overlap. RLS causes sleep onset delay due to uncomfortable sensations and urge to move legs. [6] | Check serum ferritin; low ferritin (less than 50 mcg/L) exacerbates RLS and should be repleted. |
| Cardiovascular Disease | Insomnia is associated with increased risk of hypertension, coronary artery disease, heart failure, and stroke. [20] | Chronic sleep deprivation activates sympathetic nervous system and inflammatory pathways. |
| COPD and Asthma | 40-60% of patients with COPD report insomnia, related to nocturnal dyspnoea, cough, and medication (bronchodilators). [6] | Optimize respiratory management; consider timing of bronchodilators. |
| Gastro-Oesophageal Reflux Disease (GORD) | Nocturnal reflux disrupts sleep. Common in obese patients and those with hiatus hernia. [6] | Elevate head of bed, avoid late-night meals, consider proton pump inhibitor. |
| Menopause | Up to 60% of perimenopausal and postmenopausal women report insomnia, often related to vasomotor symptoms (hot flushes). [5] | Hormone replacement therapy (HRT) may improve sleep in women with vasomotor symptoms. |
| Substance Use | Alcohol: Initially sedating but disrupts sleep architecture (reduced REM sleep, increased awakenings in second half of night). Caffeine: Delays sleep onset and reduces total sleep time. Stimulants (amphetamines, cocaine): Cause insomnia. [6] | Obtain detailed substance use history. Alcohol use disorder is common in patients self-medicating for insomnia. |
| Medications | Corticosteroids, beta-blockers, SSRIs (initial activation), theophylline, decongestants, antiepileptics (some), stimulants (methylphenidate, modafinil). [6] | Review medication history and consider timing of administration (e.g., diuretics in morning to reduce nocturia). |
3. Aetiology and Pathophysiology
Conceptual Models
Spielman's 3P Model
The Spielman 3P Model provides a framework for understanding how insomnia develops and becomes chronic. [7]
-
Predisposing Factors (Vulnerability)
- Genetic: Twin studies suggest heritability of ~40-50%. Polymorphisms in circadian clock genes (e.g., PER3, CLOCK) are associated with insomnia. [7]
- Hyperarousal Trait: Individuals with heightened physiological and cognitive arousal are predisposed to insomnia. This includes elevated resting heart rate, increased cortisol secretion, and rumination tendencies.
- Personality Traits: Perfectionism, neuroticism, tendency to worry, and rumination. [7]
- Female Sex: Hormonal fluctuations (menstrual cycle, pregnancy, menopause) increase vulnerability. [5]
- Age: Older adults have lighter, more fragmented sleep and increased prevalence of comorbid conditions. [16]
-
Precipitating Factors (Trigger)
- Stressful Life Events: Bereavement, job loss, relationship difficulties, illness, hospitalisation. [7]
- Medical Illness: Acute pain, respiratory infections, cardiac events.
- Psychiatric Illness: Onset of depression or anxiety disorder.
- Environmental Changes: Shift work, travel across time zones (jet lag), change in sleep environment (hospital admission, partner snoring).
- Medications: Introduction of activating medications (corticosteroids, SSRIs).
-
Perpetuating Factors (Maintenance)
- Maladaptive Behaviours:
- Excessive Time in Bed: Spending 9-10 hours in bed to "catch up" on sleep reduces sleep drive and sleep efficiency.
- Daytime Napping: Reduces nocturnal sleep pressure.
- Clock-Watching: Increases anxiety and performance pressure around sleep.
- Using Bed for Non-Sleep Activities: Reading, watching TV, using phone in bed weakens the stimulus-sleep association.
- Dysfunctional Beliefs About Sleep: "I must get 8 hours of sleep or I cannot function," catastrophising about consequences of poor sleep, unrealistic expectations. [7]
- Conditioned Arousal: The bed and bedroom become associated with wakefulness and anxiety rather than sleep (classical conditioning). [7]
- Caffeine and Alcohol Use: Self-medication attempts that worsen sleep architecture. [6]
- Poor Sleep Hygiene: Irregular sleep schedule, late-night exercise, stimulating activities before bed, bright light exposure.
- Maladaptive Behaviours:
CBT-I directly targets perpetuating factors, which is why it is highly effective in breaking the cycle of chronic insomnia. [8]
Hyperarousal Model
Chronic insomnia is characterised by sustained physiological, cognitive, and cortical hyperarousal that persists across 24 hours (not just at night). [7]
-
Physiological Hyperarousal:
- Elevated heart rate and heart rate variability.
- Increased whole-body metabolic rate.
- Elevated core body temperature during sleep.
- Increased cortisol secretion, particularly in the evening and early nighttime. [7]
- Increased sympathetic nervous system activation.
-
Cognitive Hyperarousal:
- Racing thoughts, worry, rumination at bedtime.
- Difficulty "switching off" the mind.
- Attention bias toward sleep-related threats and monitoring of bodily sensations. [7]
-
Cortical Hyperarousal:
- EEG studies show increased high-frequency beta activity during NREM sleep (indicating reduced depth of sleep).
- Functional neuroimaging (fMRI) demonstrates increased activity in regions associated with arousal and alertness (anterior cingulate cortex, amygdala) and reduced deactivation of the default mode network during sleep attempts. [7]
This hyperarousal model explains why patients with insomnia often do not feel sleepy despite sleep deprivation and why insomnia is associated with increased daytime alertness (paradoxically) in some individuals.
Sleep Architecture Changes in Insomnia
Polysomnographic (PSG) findings in chronic insomnia (compared to normal sleepers): [2]
| Parameter | Finding in Insomnia |
|---|---|
| Sleep Onset Latency (SOL) | Prolonged (> 30 minutes). |
| Wake After Sleep Onset (WASO) | Increased (frequent awakenings). |
| Total Sleep Time (TST) | Reduced. |
| Sleep Efficiency (SE) | Reduced (less than 85%). Calculated as (TST / Time in Bed) × 100. |
| NREM Sleep | Reduced slow-wave sleep (Stage N3), increased Stage N1 (light sleep). |
| REM Sleep | Variable; may be reduced or fragmented. |
| EEG Microstructure | Increased beta activity during NREM sleep (indicative of cortical arousal). |
Note: PSG is not routinely indicated for diagnosing insomnia unless there is suspicion of another primary sleep disorder (OSA, narcolepsy, REM behaviour disorder). [2] Insomnia is a clinical diagnosis based on history.
Neurobiological Mechanisms
Exam Detail: Neurotransmitter Systems Implicated in Insomnia:
-
GABAergic System: Reduced GABAergic inhibition in arousal-promoting regions may contribute to hyperarousal. Benzodiazepines and Z-drugs act as GABA-A receptor positive allosteric modulators, enhancing GABAergic inhibition. [12]
-
Orexinergic System: Orexin (hypocretin) neurons in the lateral hypothalamus promote wakefulness. Overactivity may contribute to insomnia. Dual orexin receptor antagonists (DORAs, e.g., suvorexant) block orexin signaling and are approved for insomnia in some countries. [21]
-
Histaminergic System: Histamine promotes wakefulness. Sedating antihistamines (e.g., diphenhydramine) block H1 receptors but have poor evidence for chronic insomnia and significant anticholinergic side effects. [12]
-
Melatonergic System: Melatonin, secreted by the pineal gland in response to darkness, promotes sleep onset and regulates circadian rhythm. Exogenous melatonin (prolonged-release formulation) is effective in older adults. [11]
-
HPA Axis Dysregulation: Chronic insomnia is associated with elevated evening and nocturnal cortisol levels, reflecting overactivation of the hypothalamic-pituitary-adrenal (HPA) axis. [7]
4. Clinical Presentation
Diagnostic Criteria (ICSD-3 and DSM-5)
Chronic Insomnia Disorder is diagnosed based on the following criteria (ICSD-3 / DSM-5): [2,3]
A. Symptoms (one or more):
- Difficulty initiating sleep (prolonged sleep onset latency).
- Difficulty maintaining sleep (frequent awakenings or difficulty returning to sleep after awakening).
- Early morning awakening with inability to return to sleep.
- Resistance to going to bed at appropriate time (in children).
- Difficulty sleeping without parent or caregiver intervention (in children).
B. Daytime Impairment (one or more):
- Fatigue or malaise.
- Attention, concentration, or memory impairment.
- Social, family, occupational, or academic impairment.
- Mood disturbance (irritability, dysphoria).
- Daytime sleepiness (though less prominent than in sleep apnoea).
- Behavioural problems (hyperactivity, impulsivity, aggression).
- Reduced motivation, energy, or initiative.
- Proneness to errors or accidents (e.g., driving).
- Concerns or dissatisfaction about sleep.
C. Frequency and Duration:
- Symptoms occur ≥3 nights per week.
- Symptoms persist for ≥3 months.
D. Adequate Opportunity:
- The individual has adequate opportunity and circumstances for sleep (i.e., not shift work, not acute hospital setting).
E. Not Better Explained by Another Sleep Disorder:
- Symptoms are not better explained by another sleep disorder (e.g., OSA, narcolepsy, circadian rhythm disorder, parasomnia).
F. Not Attributable to Substance or Medical Condition:
- Not attributable to the physiological effects of a substance (medication, drug of abuse) or another medical condition (though comorbid insomnia is common and can be diagnosed alongside medical/psychiatric conditions).
Short-Term Insomnia Disorder: Symptoms present for less than 3 months but otherwise meet criteria. [2]
Subtypes of Insomnia
| Subtype | Characteristics |
|---|---|
| Sleep Onset Insomnia | Difficulty falling asleep (sleep onset latency > 30 minutes). Often associated with anxiety, racing thoughts, or delayed sleep phase. Patient lies awake for prolonged period at bedtime. |
| Sleep Maintenance Insomnia | Difficulty staying asleep. Frequent awakenings during the night (wake after sleep onset > 30 minutes). Difficulty returning to sleep after awakening. Common in middle-aged and elderly adults. |
| Early Morning Awakening | Waking 1-2 hours (or more) before desired wake time, with inability to return to sleep. Classically associated with depression (though not specific). More common in older adults. |
| Mixed Insomnia | Combination of sleep onset, maintenance, and early awakening difficulties. Most common pattern in clinical practice. |
| Paradoxical Insomnia (Sleep State Misperception) | Subjective complaint of severe insomnia, but objective sleep measures (PSG, actigraphy) show near-normal sleep. Patient genuinely perceives poor sleep. Likely reflects heightened perception of wakefulness. [2] |
Daytime Consequences
Daytime impairment is essential for diagnosis. Common daytime symptoms include: [2,3]
| Symptom | Description |
|---|---|
| Fatigue / Tiredness | Persistent sense of tiredness, lack of energy. Feeling "unrefreshed" by sleep. |
| Cognitive Impairment | Difficulty concentrating, poor memory, reduced attention span, slowed processing speed. Impaired decision-making. |
| Mood Disturbance | Irritability, dysphoria, emotional lability, anxiety, reduced frustration tolerance. |
| Daytime Sleepiness | May be present, but is less prominent than in OSA or narcolepsy. Some patients report "tired but wired" (hyperarousal). |
| Reduced Motivation / Energy | Lack of drive, apathy, reduced interest in activities. |
| Impaired Functioning | Reduced work performance, impaired social relationships, difficulty with household tasks, increased absenteeism. |
| Increased Risk of Errors / Accidents | Slower reaction times, impaired vigilance. Increased risk of motor vehicle accidents (similar magnitude to alcohol impairment in severe insomnia). [20] |
| Physical Symptoms | Headaches, gastrointestinal symptoms, muscle tension. |
Comprehensive History Taking
A detailed sleep history is the cornerstone of diagnosis. [14]
Sleep History
| Domain | Key Questions |
|---|---|
| Sleep Schedule | What time do you go to bed? What time do you try to fall asleep? How long does it take to fall asleep (sleep onset latency)? How many times do you wake during the night? How long are you awake during the night (wake after sleep onset)? What time do you wake in the morning (final awakening)? What time do you get out of bed? Do you nap during the day? If so, when and for how long? |
| Sleep Quality | Do you feel refreshed on waking? How would you rate your sleep quality (0-10)? Do you dream? (Assesses REM sleep; absence may suggest REM suppression from alcohol or medication). |
| Variability | Does your sleep pattern differ on weekends vs. weekdays? (Suggests social jet lag or delayed sleep phase). |
| Sleep Environment | Is your bedroom dark, quiet, and cool? Is your mattress and bedding comfortable? Does your partner snore or disturb your sleep? Do you use electronic devices (phone, TV, tablet) in bed or before sleep? |
| Pre-Sleep Routine | What do you do in the hour before bed? Do you engage in stimulating activities (work, exercise, arguments)? Do you use screens? Do you consume caffeine or alcohol in the evening? |
| Sleep Behaviours | Do you watch the clock during the night? Do you lie in bed awake for long periods? Do you do non-sleep activities in bed (reading, watching TV, working)? Do you get up and leave the bedroom if unable to sleep? |
Daytime Impact Assessment
- Fatigue severity (0-10 scale).
- Impact on work, social life, relationships.
- Mood changes (irritability, low mood).
- Cognitive difficulties (concentration, memory).
- Safety concerns (driving, operating machinery).
Psychiatric and Medical History
| Domain | Assessment |
|---|---|
| Psychiatric Screening | Screen for depression (PHQ-9), anxiety (GAD-7), bipolar disorder, PTSD, OCD. Insomnia is highly comorbid with psychiatric conditions. [6] Ask about suicidal ideation (insomnia is an independent risk factor for suicide). [18] |
| Medical Comorbidities | Chronic pain (arthritis, fibromyalgia, neuropathic pain). Cardiovascular (heart failure, angina – nocturnal symptoms). Respiratory (COPD, asthma – nocturnal dyspnoea, cough). Gastrointestinal (GORD – nocturnal reflux). Urological (nocturia – frequency, BPH, overactive bladder). Endocrine (hyperthyroidism – hypermetabolic state). Neurological (Parkinson's disease, dementia, stroke). Menopause (vasomotor symptoms). |
| Medication Review | Current medications (prescription and over-the-counter). Previous hypnotic use (type, dose, duration, response, side effects). Medications that may cause insomnia: Corticosteroids, SSRIs (initial), beta-blockers (lipophilic), theophylline, decongestants, stimulants, diuretics (nocturia). |
| Substance Use | Caffeine: Quantity (cups per day), timing of last intake. Half-life ~5 hours; afternoon/evening intake disrupts sleep. [6] Alcohol: Quantity, frequency, timing. Initially sedating but disrupts sleep architecture. [6] Tobacco: Nicotine is a stimulant. Withdrawal during night can cause awakening. Illicit Drugs: Stimulants (cocaine, amphetamines, MDMA), cannabis. |
Screening for Other Sleep Disorders
| Sleep Disorder | Red Flag Symptoms | Action |
|---|---|---|
| Obstructive Sleep Apnoea (OSA) | Loud snoring, witnessed apnoeas (breathing pauses), excessive daytime sleepiness, morning headaches, obesity, large neck circumference. Use STOP-BANG questionnaire. [19] | Refer for overnight oximetry or polysomnography. Treat OSA with CPAP; insomnia may require separate treatment ("COMISA"). |
| Restless Legs Syndrome (RLS) | Urge to move legs, worse at rest/evening, relieved by movement, uncomfortable sensations in legs. Delays sleep onset. [6] | Check serum ferritin (replète if less than 50-75 mcg/L). Consider dopamine agonists (pramipexole, ropinirole) or alpha-2-delta ligands (gabapentin, pregabalin). |
| Periodic Limb Movement Disorder (PLMD) | Repetitive limb movements during sleep (often reported by bed partner). Patient may be unaware. | Diagnosed on polysomnography. Often coexists with RLS. |
| Circadian Rhythm Disorders | Delayed Sleep Phase: "Night owl" pattern, difficulty falling asleep before 2-3 AM, difficulty waking in morning, normal sleep if allowed to sleep on preferred schedule. Common in adolescents/young adults. Advanced Sleep Phase: "Early bird," falls asleep early evening, wakes very early morning. Common in elderly. Shift Work Disorder: Insomnia related to shift work schedule. [2] | Sleep diary, actigraphy. Bright light therapy, melatonin. Chronotherapy (gradual shifting of sleep schedule). |
| Narcolepsy | Excessive daytime sleepiness (sudden, irresistible sleep attacks), cataplexy (sudden muscle weakness triggered by emotion), sleep paralysis, hypnagogic/hypnopompic hallucinations. [2] | Refer to sleep specialist. Multiple Sleep Latency Test (MSLT). |
| REM Behaviour Disorder (RBD) | Dream enactment behaviours (acting out dreams), vocalisation, violent movements during sleep. Loss of normal REM atonia. Risk of injury. Associated with synucleinopathies (Parkinson's, Lewy body dementia). [2] | Refer to sleep specialist. PSG shows REM without atonia. Treat with melatonin or clonazepam. Screen for neurodegenerative disease. |
Partner / Collateral History
A bed partner history is invaluable for identifying unrecognised sleep disorders:
- Snoring, witnessed apnoeas (OSA).
- Leg movements, kicking (RLS, PLMD).
- Vocalisation, dream enactment (RBD).
- Sleep schedule, napping.
5. Differential Diagnosis
Insomnia is a symptom that can arise from multiple causes. The differential diagnosis includes:
| Diagnosis | Key Distinguishing Features |
|---|---|
| Primary Chronic Insomnia Disorder | Difficulty initiating/maintaining sleep ≥3 nights/week for ≥3 months. Daytime impairment. No other sleep disorder, medical, or psychiatric cause fully explains symptoms (though comorbidities may coexist). |
| Depression-Related Insomnia | Early morning awakening (classic, though not universal). Low mood, anhedonia, reduced energy, appetite/weight changes, guilt, suicidal ideation. Treat underlying depression (antidepressants, psychotherapy); insomnia often improves but may require CBT-I. [6,18] |
| Anxiety Disorder-Related Insomnia | Sleep onset insomnia (difficulty initiating sleep due to racing thoughts, worry, rumination). Daytime anxiety symptoms. Treat anxiety (CBT, SSRIs); CBT-I may be needed. [6] |
| Bipolar Disorder | Reduced need for sleep (not insomnia) during manic/hypomanic episodes (feels rested after 2-3 hours). Insomnia may occur in depressive episodes. Screen for manic/hypomanic episodes. [3] |
| Obstructive Sleep Apnoea (OSA) | Loud snoring, witnessed apnoeas, excessive daytime sleepiness (prominent), gasping/choking during sleep, morning headaches, obesity, large neck circumference. May have insomnia symptoms (especially sleep maintenance). STOP-BANG score ≥3. [19] Refer for sleep study (overnight oximetry or PSG). Treat with CPAP. |
| Restless Legs Syndrome (RLS) | Urge to move legs, worse at rest/evening, relieved by movement. Uncomfortable sensations (crawling, tingling) in legs. Sleep onset delay. Check ferritin (low ferritin exacerbates RLS). [6] Treat with iron repletion, dopamine agonists, or alpha-2-delta ligands. |
| Periodic Limb Movement Disorder (PLMD) | Repetitive limb movements during sleep (often legs). Patient may be unaware; bed partner reports kicking. Diagnosed on PSG. Often coexists with RLS. |
| Circadian Rhythm Sleep-Wake Disorders | Delayed Sleep Phase Disorder (DSPD): Cannot fall asleep until late (2-3 AM), difficulty waking, normal sleep if allowed to sleep on preferred schedule. Common in adolescents/young adults. Advanced Sleep Phase Disorder (ASPD): Falls asleep early evening, wakes very early morning. Common in elderly. Shift Work Disorder: Insomnia related to work schedule. [2] Sleep diary and actigraphy confirm circadian misalignment. Treat with bright light therapy, melatonin, chronotherapy. |
| Narcolepsy | Excessive daytime sleepiness (sudden, irresistible sleep attacks) is cardinal feature. Cataplexy (sudden muscle weakness triggered by emotion – pathognomonic), sleep paralysis, hypnagogic/hypnopompic hallucinations. Disturbed nocturnal sleep may occur. [2] Refer to sleep specialist. MSLT shows short sleep latency and early REM. |
| Substance-Induced Sleep Disorder | Caffeine: Delays sleep onset, reduces total sleep time. Half-life ~5 hours. [6] Alcohol: Initially sedating but disrupts sleep architecture (suppresses REM, increases awakenings in second half of night). Chronic use causes insomnia. Withdrawal causes severe insomnia. [6] Stimulants (amphetamines, cocaine, MDMA, modafinil, methylphenidate): Cause insomnia. Nicotine: Stimulant; withdrawal during night causes awakening. |
| Medication-Induced Insomnia | Corticosteroids: Cause hyperarousal, insomnia. SSRIs/SNRIs: Initial activation may worsen insomnia (usually transient). Beta-blockers (lipophilic, e.g., propranolol): Suppress melatonin, cause nightmares. Theophylline: Stimulant. Decongestants (pseudoephedrine): Stimulant. Diuretics: Nocturia. [6] Review medication list; consider timing of administration or alternative agents. |
| Medical Condition-Related Insomnia | Chronic Pain (arthritis, fibromyalgia, neuropathic pain): Pain disrupts sleep; sleep deprivation lowers pain threshold (bidirectional). [6] Heart Failure: Orthopnoea, paroxysmal nocturnal dyspnoea. COPD/Asthma: Nocturnal dyspnoea, cough. Bronchodilators may worsen insomnia. [6] GORD: Nocturnal reflux, heartburn. Nocturia: BPH, overactive bladder, diabetes, diuretics. Hyperthyroidism: Hypermetabolic state, anxiety. Menopause: Vasomotor symptoms (hot flushes, night sweats). [5] Neurodegenerative Diseases (Parkinson's, dementia): Sleep fragmentation, RBD. Treat underlying medical condition. |
| Parasomnias | REM Behaviour Disorder: Dream enactment, vocalisation, movements during REM sleep. Risk of injury. Associated with synucleinopathies. [2] Sleepwalking, Sleep Terrors: Arousal from NREM sleep. Common in children; may persist or emerge in adults. Nightmare Disorder: Frequent nightmares (REM-related). Associated with PTSD, stress. |
| Psychophysiological Insomnia (Learned Insomnia) | Conditioned arousal to sleep environment. Heightened anxiety and cognitive arousal when attempting to sleep. Sleeps better away from home (e.g., hotel). Responds well to CBT-I (stimulus control, cognitive therapy). [7] |
| Paradoxical Insomnia (Sleep State Misperception) | Severe subjective insomnia complaint, but objective measures (PSG, actigraphy) show near-normal sleep. Patient genuinely perceives poor sleep. Reflects heightened perception of wakefulness. Responds to CBT-I (cognitive restructuring). [2] |
6. Investigations
Insomnia is a clinical diagnosis based on history. Routine laboratory tests or polysomnography are not required for uncomplicated insomnia. [14] Investigations are indicated when:
- There is suspicion of another primary sleep disorder (OSA, narcolepsy, RLS).
- There is suspicion of an underlying medical condition contributing to insomnia.
- Initial treatment has failed and re-evaluation is needed.
Essential Assessment Tools
| Tool | Purpose | Details |
|---|---|---|
| Sleep Diary | Gold standard for assessing sleep patterns over time. Prospective, patient-completed record. [14] | Patient records daily for 2 weeks: Bedtime, time attempting to fall asleep, estimated sleep onset latency, number and duration of awakenings, final wake time, out-of-bed time, total sleep time, naps, daytime functioning, caffeine/alcohol use, medication use. Reveals patterns, variability, sleep efficiency. Essential for diagnosis and monitoring treatment response. |
| Insomnia Severity Index (ISI) | Brief, validated 7-item questionnaire assessing severity of insomnia symptoms and daytime impact. [14] | Score 0-7: No insomnia. 8-14: Subthreshold insomnia. 15-21: Moderate insomnia. 22-28: Severe insomnia. Useful for screening and monitoring treatment response. |
| Epworth Sleepiness Scale (ESS) | Assesses daytime sleepiness (8-item questionnaire). [14] | Score > 10 suggests excessive daytime sleepiness and raises suspicion for OSA or narcolepsy rather than primary insomnia (insomnia typically causes fatigue, not excessive sleepiness). Refer for sleep study if ESS > 10 and clinical suspicion of OSA. |
| PHQ-9 (Depression) | Screen for major depressive disorder. [18] | 9-item questionnaire. Score ≥10 suggests depression. Insomnia is a symptom of depression and a risk factor for depression. |
| GAD-7 (Anxiety) | Screen for generalized anxiety disorder. [6] | 7-item questionnaire. Score ≥10 suggests anxiety disorder. Anxiety commonly causes insomnia (sleep onset difficulty). |
| STOP-BANG Questionnaire | Screen for obstructive sleep apnoea. [19] | 8 yes/no questions: Snoring, Tiredness, Observed apnoeas, Pressure (hypertension), BMI > 35, Age > 50, Neck circumference > 40 cm, Gender (male). Score ≥3 suggests high risk for OSA; refer for sleep study. |
Investigations to Consider
| Investigation | Indication | Interpretation |
|---|---|---|
| Actigraphy | Objective assessment of sleep-wake patterns over 1-2 weeks. Wrist-worn accelerometer measures movement. [14] | Provides objective data on sleep onset, wake time, total sleep time, sleep efficiency. Useful for circadian rhythm disorders (delayed/advanced sleep phase, shift work disorder). Correlation with PSG is moderate (overestimates sleep in insomnia). Not a substitute for PSG for diagnosing OSA or narcolepsy. Less detailed than sleep diary but objective. |
| Polysomnography (PSG) | Overnight sleep study in sleep laboratory. NOT routinely indicated for insomnia. [2,14] | Indications: Suspicion of OSA (snoring, apnoeas, excessive daytime sleepiness). Suspicion of narcolepsy (followed by MSLT). Suspicion of REM Behaviour Disorder (dream enactment). Suspicion of PLMD. Treatment-refractory insomnia (to exclude undiagnosed sleep disorder). Findings in insomnia (if PSG performed): Prolonged sleep onset latency, increased wake after sleep onset, reduced total sleep time, reduced sleep efficiency, increased Stage N1, reduced Stage N3 (slow-wave sleep), increased beta activity on EEG. |
| Multiple Sleep Latency Test (MSLT) | Daytime sleep study to assess for narcolepsy or idiopathic hypersomnia. [2] | Performed the day after PSG. Patient attempts to nap at 2-hour intervals (5 naps total). Measures sleep onset latency and presence of REM sleep. Narcolepsy: Mean sleep latency less than 8 minutes, ≥2 sleep-onset REM periods (SOREMPs). Not indicated for insomnia. |
| Blood Tests | Not routine. Consider if underlying medical cause suspected. | TFTs (thyroid function): Hyperthyroidism causes insomnia (hypermetabolic state, anxiety). Serum Ferritin: Low ferritin (less than 50-75 mcg/L) exacerbates RLS; replète with oral iron. [6] HbA1c / Fasting Glucose: Diabetes may cause nocturia (polyuria). U&Es: Chronic kidney disease may cause nocturia, RLS (uraemia). FBC: Anaemia may cause fatigue (though not insomnia per se). LFTs: Liver disease may cause pruritus (disrupts sleep). |
| ECG | If suspicion of cardiac arrhythmia or cardiac cause of nocturnal symptoms. | Atrial fibrillation, ventricular arrhythmias may cause nocturnal palpitations or dyspnoea. |
| Urine Analysis / Post-Void Residual | If nocturia is prominent. | Exclude urinary tract infection, diabetes (glycosuria), bladder outlet obstruction (BPH in men). |
7. Management
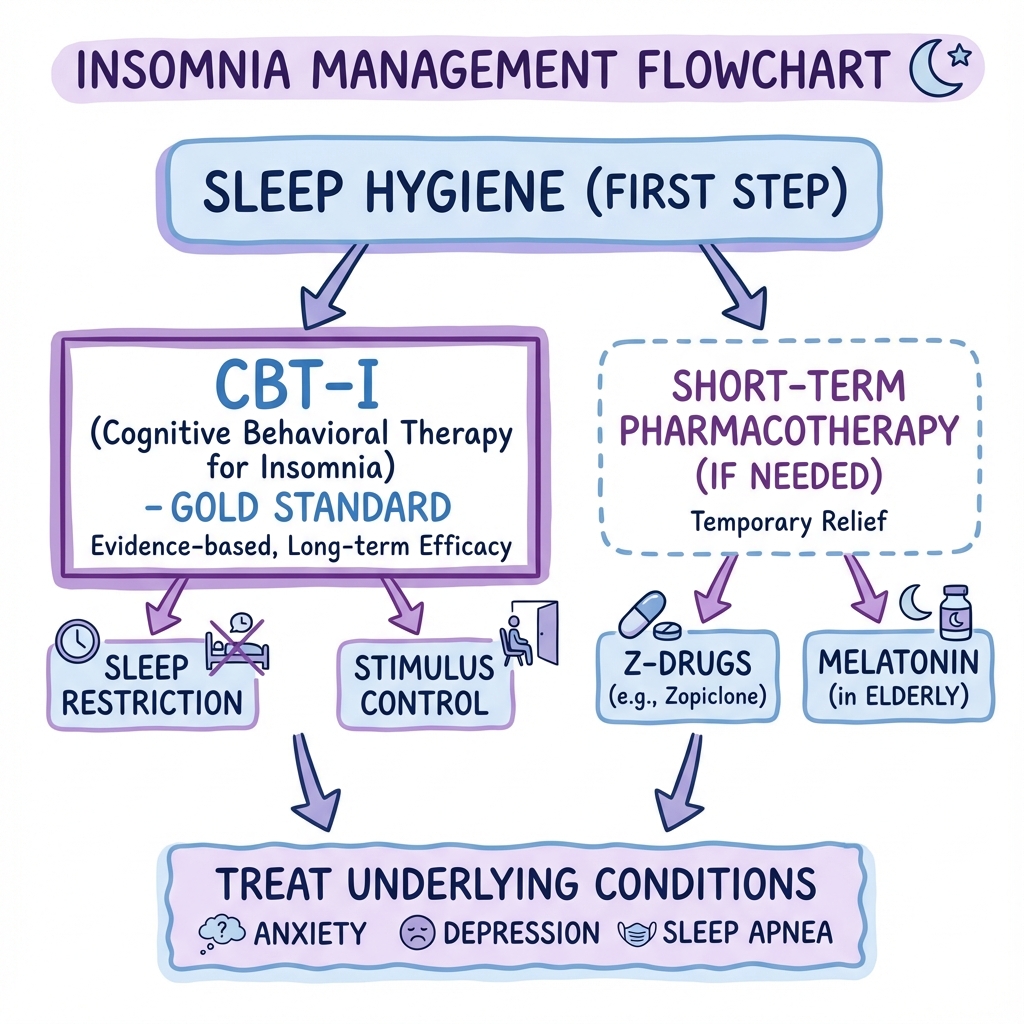
Management of chronic insomnia is multimodal and prioritises non-pharmacological interventions. [8,9,11]
General Principles
- CBT-I is First-Line Treatment: Cognitive Behavioural Therapy for Insomnia has the strongest evidence for efficacy and durability. [8,9]
- Identify and Treat Comorbidities: Address psychiatric (depression, anxiety), medical (pain, OSA, RLS), and substance use issues. [6]
- Pharmacotherapy is Short-Term Adjunct: Hypnotics should be used for short-term only (2-4 weeks maximum) when CBT-I is unavailable or as adjunct during acute exacerbations. [11,12]
- Avoid Long-Term Hypnotic Use: Risk of tolerance, dependence, rebound insomnia, falls, cognitive impairment. [12]
- Patient Education: Explain sleep physiology, realistic expectations (total sleep time decreases with age), and the chronic, fluctuating nature of insomnia.
Management Algorithm
PATIENT PRESENTING WITH INSOMNIA
(Difficulty Initiating / Maintaining Sleep + Daytime Impairment)
↓
COMPREHENSIVE SLEEP HISTORY + COMORBIDITY SCREEN
- Sleep diary (2 weeks)
- ISI, PHQ-9, GAD-7, STOP-BANG
- Medical, psychiatric, substance use history
↓
MEET CRITERIA FOR CHRONIC INSOMNIA DISORDER?
(≥3 nights/week for ≥3 months)
↙ ↘
YES NO
↓ ↓
SHORT-TERM INSOMNIA (less than 3 months)
- Identify and address precipitant
↓ - Sleep hygiene education
- Short-term CBT-I or hypnotic (if needed)
EXCLUDE / TREAT OTHER SLEEP DISORDERS ↓
- OSA (STOP-BANG ≥3 → Sleep study) REASSESS IN 4-6 WEEKS
- RLS (Ferritin, dopamine agonists)
- Circadian rhythm disorder (Sleep diary, actigraphy)
- Narcolepsy (ESS > 10, MSLT)
↓
IDENTIFY AND TREAT COMORBID CONDITIONS
- Depression (Antidepressants, psychotherapy)
- Anxiety (CBT, SSRIs)
- Chronic Pain (Analgesia, physiotherapy)
- Medical Conditions (Optimize management)
- Substance Use (Reduce caffeine/alcohol, cessation support)
- Medication Review (Timing, alternatives)
↓
SLEEP HYGIENE EDUCATION (For All Patients)
┌──────────────────────────────────────────────────────────────┐
│ - Consistent bed and wake times (including weekends) │
│ - Avoid caffeine after noon (half-life ~5 hours) │
│ - Avoid alcohol (disrupts sleep architecture) │
│ - Avoid screens 1 hour before bed (blue light suppresses │
│ melatonin; cognitive stimulation) │
│ - Create optimal sleep environment: dark, quiet, cool │
│ (16-19°C ideal), comfortable bed │
│ - Regular exercise (at least 4 hours before bed) │
│ - Avoid large meals, heavy fluids close to bedtime │
│ - Relaxing pre-sleep routine (reading, bath, relaxation) │
│ - Avoid clock-watching (turn clock away) │
│ - Limit daytime naps (less than 30 mins, before 3 PM if needed) │
│ - Use bed for sleep and sex only (not reading, TV, work) │
└──────────────────────────────────────────────────────────────┘
↓
FIRST-LINE: COGNITIVE BEHAVIOURAL THERAPY FOR INSOMNIA (CBT-I)
┌──────────────────────────────────────────────────────────────┐
│ GOLD STANDARD TREATMENT [8,9] │
│ - Format: Individual, group, or digital (e.g., Sleepio) │
│ - Duration: 4-8 sessions (weekly or biweekly) │
│ - Evidence: 70-80% response rate; durable effects (1-2 yrs) │
│ │
│ COMPONENTS: │
│ │
│ 1. SLEEP RESTRICTION THERAPY │
│ - Limit time in bed to match actual sleep time │
│ - Calculate sleep efficiency (SE) from sleep diary: │
│ SE = (Total Sleep Time / Time in Bed) × 100 │
│ - Prescribe time in bed = Total Sleep Time + 30 mins │
│ (minimum 5 hours for safety) │
│ - Fixed wake time (most important) │
│ - Gradually extend time in bed as SE improves (≥85%) │
│ - Increases sleep drive (homeostatic pressure) │
│ │
│ 2. STIMULUS CONTROL THERAPY │
│ - Bed and bedroom for sleep and sex ONLY │
│ - Go to bed only when sleepy (not tired) │
│ - If unable to sleep within 15-20 mins, get up and leave │
│ bedroom (return when sleepy) │
│ - Avoid reading, TV, phone, work in bed │
│ - Same wake time every day (including weekends) │
│ - Avoid daytime napping │
│ - Strengthens bed-sleep association (classical │
│ conditioning) [7] │
│ │
│ 3. COGNITIVE THERAPY │
│ - Identify and challenge dysfunctional beliefs about │
│ sleep [7] │
│ - Examples: "I must get 8 hours or I cannot function," │
│ "Insomnia will ruin my health," "I will never sleep │
│ well again" │
│ - Restructure catastrophic thinking │
│ - Address performance anxiety around sleep │
│ - Realistic expectations (sleep need decreases with age) │
│ │
│ 4. RELAXATION TRAINING │
│ - Progressive muscle relaxation (PMR) │
│ - Diaphragmatic breathing │
│ - Mindfulness meditation │
│ - Guided imagery │
│ - Reduces physiological and cognitive arousal [7] │
│ │
│ 5. SLEEP HYGIENE EDUCATION │
│ - Consistent schedule, environment, avoid stimulants │
│ │
│ DIGITAL CBT-I: │
│ - Sleepio (NICE-approved, UK NHS available) [10] │
│ - SHUTi, Somryst (FDA-approved, USA) │
│ - Efficacy comparable to face-to-face CBT-I [10] │
│ - Addresses access barriers │
└──────────────────────────────────────────────────────────────┘
↓
CBT-I EFFECTIVE?
↓
YES → MAINTAIN GAINS, MONITOR FOR RELAPSE
↓
NO (or CBT-I unavailable / patient declines)
↓
SHORT-TERM PHARMACOTHERAPY (ADJUNCT OR INTERIM)
┌──────────────────────────────────────────────────────────────┐
│ PRINCIPLES: │
│ - Use for SHORT-TERM ONLY (2-4 weeks max) [11,12] │
│ - Intermittent dosing (3-4 nights/week) preferred over │
│ nightly to reduce tolerance and dependence [12] │
│ - Lowest effective dose │
│ - Taper gradually to avoid rebound insomnia │
│ - Combine with CBT-I when possible │
│ - Avoid long-term use (> 4 weeks continuous) │
│ │
│ OPTIONS: │
│ │
│ 1. Z-DRUGS (Non-Benzodiazepine Hypnotics) │
│ - ZOPICLONE 3.75-7.5 mg nocte │
│ • Short-acting (half-life ~5 hours) │
│ • Side effects: Metallic taste, next-day sedation │
│ - ZOLPIDEM 5-10 mg nocte │
│ • Very short-acting (half-life ~2.5 hours) │
│ • Preferred for sleep onset insomnia │
│ - Mechanism: GABA-A receptor positive allosteric │
│ modulators (selective for α1 subunit) [12] │
│ - Risks: Tolerance, dependence (similar to BZDs), │
│ next-day sedation, falls (elderly), cognitive │
│ impairment, rare parasomnias (sleepwalking, sleep │
│ driving) [12] │
│ - Caution in elderly (start 3.75 mg zopiclone, 5 mg │
│ zolpidem), avoid in severe respiratory disease, hepatic │
│ impairment, myasthenia gravis │
│ │
│ 2. SHORT-ACTING BENZODIAZEPINES │
│ - TEMAZEPAM 10-20 mg nocte │
│ • Half-life ~8-15 hours (intermediate) │
│ - LORMETAZEPAM 0.5-1.5 mg nocte (UK) │
│ • Half-life ~10 hours │
│ - Mechanism: GABA-A receptor positive allosteric │
│ modulators (non-selective) [12] │
│ - Risks: Similar to Z-drugs. AVOID long-acting BZDs │
│ (diazepam, flurazepam) due to accumulation and hangover │
│ - Avoid in elderly (increased fall risk), respiratory │
│ disease, alcohol use │
│ │
│ 3. MELATONIN (Prolonged-Release) │
│ - CIRCADIN (Melatonin PR) 2 mg nocte, 1-2 hours before │
│ bed │
│ - Licensed for PRIMARY INSOMNIA in patients ≥55 years │
│ (UK, Europe) [11] │
│ - Duration: Up to 13 weeks │
│ - Mechanism: MT1/MT2 melatonin receptor agonist; │
│ promotes sleep onset, regulates circadian rhythm [11] │
│ - Evidence: Modest improvement in sleep onset latency │
│ and quality in older adults [11] │
│ - Lower abuse potential, no withdrawal, minimal side │
│ effects (headache, dizziness) │
│ - Preferred in elderly over BZDs/Z-drugs (safer) │
│ - Caution: Interacts with CYP1A2 (fluvoxamine increases │
│ levels), warfarin (monitor INR) │
│ │
│ 4. LOW-DOSE SEDATING ANTIDEPRESSANTS (Off-Label) │
│ - AMITRIPTYLINE 10-25 mg nocte │
│ • Tricyclic antidepressant (TCA) │
│ • Sedating (H1, muscarinic antagonism) │
│ • Side effects: Dry mouth, constipation, urinary │
│ retention, postural hypotension, QTc prolongation │
│ • Caution in elderly (anticholinergic burden, falls) │
│ • Avoid in cardiac disease (arrhythmia risk) │
│ - MIRTAZAPINE 7.5-15 mg nocte │
│ • Noradrenergic and specific serotonergic │
│ antidepressant (NaSSA) │
│ • Sedating (H1 antagonism; more sedating at lower doses)│
│ • Side effects: Weight gain, increased appetite │
│ • Better tolerated than TCAs in elderly │
│ - TRAZODONE 25-50 mg nocte │
│ • Serotonin antagonist and reuptake inhibitor (SARI) │
│ • Sedating (H1, α1 antagonism) │
│ • Side effects: Postural hypotension, priapism (rare) │
│ - Consider in patients with COMORBID DEPRESSION or │
│ refractory insomnia [6] │
│ - Off-label use; limited evidence for primary insomnia │
│ │
│ 5. DUAL OREXIN RECEPTOR ANTAGONISTS (DORAs) │
│ - SUVOREXANT (USA, Japan; not UK) │
│ - Mechanism: Block orexin (hypocretin) signaling, │
│ reducing wakefulness [21] │
│ - Evidence: Effective for sleep onset and maintenance │
│ - Lower abuse potential than BZDs/Z-drugs │
│ - Not widely available; expensive │
│ │
│ AGENTS TO AVOID: │
│ - Sedating antihistamines (diphenhydramine, promethazine): │
│ Tolerance develops rapidly; anticholinergic side effects │
│ (confusion, urinary retention, constipation in elderly); │
│ poor evidence [12] │
│ - Long-acting benzodiazepines (diazepam, flurazepam): │
│ Accumulation, next-day sedation, falls [12] │
│ - Antipsychotics (quetiapine, olanzapine): Off-label for │
│ insomnia; metabolic side effects (weight gain, diabetes); │
│ reserve for severe refractory cases or psychotic disorders │
└──────────────────────────────────────────────────────────────┘
↓
INADEQUATE RESPONSE TO CBT-I + SHORT-TERM PHARMACOTHERAPY?
↓
REASSESS AND REFER TO SPECIALIST
┌──────────────────────────────────────────────────────────────┐
│ - Review diagnosis: Undiagnosed sleep disorder (OSA, RLS)? │
│ - Review comorbidities: Untreated depression, anxiety, pain? │
│ - Review adherence to CBT-I │
│ - Consider actigraphy or PSG │
│ - Refer to SLEEP MEDICINE or PSYCHIATRY │
│ - Consider specialist interventions: │
│ - Intensive CBT-I │
│ - Mindfulness-based therapy │
│ - Acceptance and Commitment Therapy (ACT) │
│ - Off-label pharmacotherapy (low-dose sedating │
│ antidepressants, DORAs if available) │
└──────────────────────────────────────────────────────────────┘
CBT-I: Detailed Components
Exam Detail: Sleep Restriction Therapy:
- Paradoxically, restricting time in bed increases sleep efficiency by building sleep drive (homeostatic pressure). [8]
- Protocol:
- Calculate average total sleep time (TST) from sleep diary.
- Prescribe time in bed (TIB) = TST + 30 minutes (minimum 5 hours for safety).
- Set fixed wake time (e.g., 7:00 AM).
- Calculate bedtime = wake time - TIB (e.g., if TIB = 6 hours, bedtime = 1:00 AM).
- Patient must get out of bed at wake time regardless of sleep quality.
- After 1 week, recalculate sleep efficiency: SE = (TST / TIB) × 100.
- If SE ≥85%, increase TIB by 15-30 minutes. If SE less than 80%, decrease TIB by 15-30 minutes. If SE 80-85%, maintain TIB.
- Repeat weekly adjustments until optimal sleep achieved.
- Initially challenging (increased daytime sleepiness); warn patient. Daytime napping is discouraged.
- Contraindicated in bipolar disorder (sleep deprivation may precipitate mania), seizure disorder (lowers seizure threshold), safety-critical occupations during initial phase.
Stimulus Control Therapy:
- Aims to re-associate bed and bedroom with sleep (not wakefulness/anxiety). [7,8]
- Instructions:
- Go to bed only when sleepy (not just tired).
- Use bed for sleep and sex only (no reading, TV, phone, eating, work).
- If unable to fall asleep within 15-20 minutes, get up and leave bedroom. Engage in quiet, non-stimulating activity (reading, listening to calm music) in dim light. Return to bed when sleepy. Repeat as needed.
- Wake at same time every morning (including weekends).
- Avoid daytime napping.
- Rationale: Breaks conditioned arousal to bed. Strengthens bed-sleep association.
Cognitive Therapy:
- Identifies and challenges unhelpful thoughts about sleep. [7,8]
- Common dysfunctional beliefs:
- "I must get 8 hours of sleep or I cannot function."
- "One bad night ruins the next day."
- "Insomnia will damage my health."
- "I will never sleep well again."
- Techniques:
- Socratic questioning: "What is the evidence for this belief?"
- Behavioural experiments: Test predictions (e.g., "If I sleep 5 hours, can I still function?").
- "Normalisation: Educate on normal sleep variability and age-related changes."
- "Mindfulness: Accept sleep variability without judgment."
- Reduces performance anxiety and catastrophising.
Relaxation Training:
- Reduces physiological and cognitive arousal. [8]
- Techniques:
- "Progressive Muscle Relaxation (PMR): Systematically tense and relax muscle groups."
- "Diaphragmatic Breathing: Slow, deep breathing (4-7-8 technique: inhale 4 seconds, hold 7 seconds, exhale 8 seconds)."
- "Mindfulness Meditation: Focus on breath, body sensations, or sounds without judgment."
- "Guided Imagery: Visualise calming scenes."
- "Autogenic Training: Self-hypnosis focusing on warmth and heaviness."
- Practiced during day and before bed. Not a "quick fix"; requires regular practice.
Special Populations
Elderly Patients
- Higher Prevalence: Chronic insomnia affects 12-20% of adults ≥65 years. [16]
- Age-Related Changes: Lighter, more fragmented sleep. Reduced slow-wave sleep. Advanced sleep phase (early bedtime, early waking). [16]
- Comorbidities: Increased medical comorbidities (pain, nocturia, cardiac, respiratory), neurodegenerative diseases (dementia, Parkinson's), polypharmacy.
- Management:
- CBT-I is effective and safe. [16]
- Melatonin (Circadin 2 mg) is preferred pharmacotherapy (safer than BZDs/Z-drugs). [11]
- "Avoid benzodiazepines and Z-drugs: High risk of falls, fractures, cognitive impairment, delirium. [12,16]"
- If hypnotic needed, use lowest dose, short-term only. Consider low-dose mirtazapine (7.5 mg) if comorbid depression.
- Address nocturia (timed diuretics, treat BPH, limit evening fluids).
- Screen for sleep apnoea (common in elderly).
Pregnant Women
- Common: Up to 80% of pregnant women report sleep disturbance, particularly in third trimester. [5]
- Causes: Hormonal changes, nocturia, back pain, leg cramps, restless legs (iron deficiency), gastro-oesophageal reflux, fetal movements, anxiety.
- Management:
- Sleep hygiene, CBT-I (safe and effective).
- Left lateral position (improves venous return, reduces aortocaval compression).
- Pregnancy pillow for support.
- Address RLS (check ferritin, replète if low; avoid dopamine agonists in pregnancy; consider low-dose clonazepam if severe).
- "Avoid pharmacotherapy if possible. If essential, short-term use of lowest dose. Benzodiazepines and Z-drugs: Category D (risk to fetus; avoid in first trimester; neonatal withdrawal, floppy baby syndrome if used near term). Melatonin: Limited safety data. Sedating antihistamines (e.g., promethazine): Category A in Australia, but limited efficacy. Consult obstetric team."
Shift Workers
- Shift Work Disorder: Insomnia or excessive sleepiness related to work schedule that overlaps usual sleep period. [2]
- Prevalence: Affects 10-40% of shift workers. [17]
- Management:
- "Sleep hygiene: Consistent sleep schedule on days off, dark and quiet bedroom, blackout curtains for daytime sleep, avoid caffeine near end of shift."
- "Melatonin: 2-3 mg before daytime sleep (after night shift) may improve sleep quality. [11]"
- "Bright Light Therapy: Exposure to bright light during shift (improves alertness); avoid bright light on commute home (wear sunglasses). [17]"
- "Strategic Napping: Short nap (20-30 mins) before shift or during break (not at end of shift)."
- "Modafinil or armodafinil: Wakefulness-promoting agents; may be used for excessive sleepiness in shift work disorder (off-label; specialist prescription). [17]"
- CBT-I adapted for shift workers.
8. Complications
Chronic insomnia is associated with significant morbidity and increased risk of multiple adverse outcomes.
| Complication | Evidence / Mechanism |
|---|---|
| Major Depressive Disorder | Insomnia is an independent risk factor for incident depression (RR ~2.0). [18] Bidirectional relationship. Persistent insomnia after treatment of depression predicts relapse. |
| Anxiety Disorders | Insomnia increases risk of developing anxiety disorders. [6] Chronic sleep deprivation heightens amygdala reactivity and impairs prefrontal regulation of emotion. |
| Suicide Risk | Insomnia is an independent risk factor for suicidal ideation and suicide attempts, even after adjusting for depression. [18] Mechanisms: Impaired problem-solving, emotional dysregulation, hopelessness. |
| Cognitive Impairment | Chronic insomnia impairs attention, concentration, working memory, processing speed, executive function. [20] Daytime functioning (work, social, academic) is reduced. |
| Cardiovascular Disease | Chronic insomnia is associated with increased risk of hypertension (RR ~1.4), coronary artery disease (RR ~1.5), heart failure, and stroke. [20] Mechanisms: Sympathetic overactivation, HPA axis dysregulation, systemic inflammation (elevated CRP, IL-6), endothelial dysfunction. |
| Metabolic Dysfunction | Chronic sleep deprivation is associated with insulin resistance, impaired glucose tolerance, increased risk of type 2 diabetes (RR ~1.3). [20] Mechanisms: Increased cortisol, reduced leptin, increased ghrelin (appetite dysregulation), weight gain. |
| Impaired Immune Function | Sleep deprivation impairs cellular immunity (reduced T-cell and NK cell function). Increased susceptibility to infections. [20] |
| Falls and Fractures | Particularly in elderly using hypnotics (benzodiazepines, Z-drugs). [12,16] Next-day sedation, impaired balance, cognitive slowing. Risk of hip fracture increased by ~50% with chronic hypnotic use in elderly. |
| Motor Vehicle Accidents | Insomnia impairs vigilance, reaction time, and decision-making. Risk of motor vehicle accidents increased (similar magnitude to alcohol impairment in severe insomnia). [20] Drowsy driving is a major public health concern. |
| Substance Misuse | Self-medication with alcohol, over-the-counter sedatives, or illicit substances. Risk of alcohol use disorder increased. [6] |
| Reduced Quality of Life | Chronic insomnia significantly impairs health-related quality of life (physical, emotional, social domains). [4] |
| Increased Healthcare Utilisation | Higher rates of primary care and specialist consultations, emergency department visits, hospitalisations. [4] |
| Work Productivity Loss | Absenteeism, presenteeism (reduced productivity while at work), increased errors, increased workplace accidents. [4] Significant economic burden. |
9. Prognosis and Outcomes
Natural History
- Chronic, Fluctuating Course: Insomnia often follows a waxing and waning pattern over years. Approximately 40-50% of patients with chronic insomnia continue to have symptoms 1-2 years later without treatment. [4]
- Persistence: Untreated chronic insomnia is highly persistent. Only ~20% achieve spontaneous remission. [4]
- Relapse: Even after successful treatment, relapse is common (30-40% over 1-2 years). Booster CBT-I sessions may be needed. [13]
Treatment Outcomes
CBT-I
- Response Rate: 70-80% of patients achieve clinically significant improvement (reduction in ISI score ≥7 points, or sleep efficiency ≥85%). [8,9,13]
- Remission Rate: ~40-50% achieve full remission (ISI score less than 8). [13]
- Durability: Effects are maintained at 1-2 year follow-up without ongoing treatment. [13] Significantly superior to pharmacotherapy in long-term outcomes.
- Effect Size: Large effect sizes for sleep onset latency (Cohen's d ~0.8-1.0), wake after sleep onset (d ~0.7-0.9), and sleep efficiency (d ~0.8). [9]
- Combination Therapy: CBT-I + pharmacotherapy may have additive short-term benefit, but long-term outcomes are similar to CBT-I alone. [9]
Pharmacotherapy
- Short-Term Efficacy: Benzodiazepines and Z-drugs reduce sleep onset latency by 10-20 minutes and increase total sleep time by 20-40 minutes compared to placebo. [12] Effect sizes are modest (Cohen's d ~0.3-0.5).
- Tolerance: Develops within 2-4 weeks of continuous use. Efficacy diminishes. [12]
- Rebound Insomnia: Upon discontinuation, transient worsening of insomnia occurs (lasting days to weeks). [12] Taper gradually to minimize rebound.
- Long-Term Outcomes: Poor. Symptoms typically return after discontinuation. [12] No evidence of sustained benefit beyond 4 weeks.
- Melatonin: Modest efficacy in older adults. Reduces sleep onset latency by ~7-10 minutes. [11] Well-tolerated, no dependence.
Prognostic Factors
Favorable Prognosis:
- Adherence to CBT-I.
- Short duration of insomnia (less than 1 year).
- Absence of severe comorbid psychiatric disorder.
- Absence of chronic pain.
- Young age.
Poor Prognosis:
- Long duration of insomnia (> 5 years).
- Comorbid major depression or anxiety disorder.
- Chronic pain syndromes.
- Chronic hypnotic use (> 1 year).
- Poor adherence to treatment.
- Severe psychophysiological arousal.
Mortality
- Cardiovascular Mortality: Some evidence suggests increased cardiovascular mortality in chronic insomnia, though findings are inconsistent. [20] Likely mediated by hypertension, inflammation, and metabolic dysfunction.
- All-Cause Mortality: Chronic use of hypnotics (benzodiazepines, Z-drugs) is associated with increased all-cause mortality (HR ~1.3-1.5), though causality is uncertain (confounding by comorbid conditions). [12]
10. Evidence and Guidelines
Key Clinical Guidelines
| Organisation | Guideline | Year | Key Recommendations |
|---|---|---|---|
| European Sleep Research Society (ESRS) | European guideline for the diagnosis and treatment of insomnia [1] | 2017 | CBT-I is first-line treatment (strong recommendation). Pharmacotherapy (BZDs, Z-drugs) for short-term use only (2-4 weeks) if CBT-I unavailable or ineffective. Avoid long-term hypnotic use. |
| American College of Physicians (ACP) | Management of Chronic Insomnia Disorder in Adults [8] | 2016 | Strong recommendation for CBT-I as initial treatment for chronic insomnia. Clinicians should discuss benefits and harms of pharmacotherapy before initiation (weak recommendation). |
| British Association for Psychopharmacology (BAP) | Evidence-based guidelines for treating insomnia [11] | 2019 | CBT-I is first-line. Short-term hypnotics (Z-drugs, melatonin ≥55 years) if needed. Avoid long-term use. Address comorbidities. |
| National Institute for Health and Care Excellence (NICE) | Guidance on insomnia (various pathways) | Various | Sleep hygiene education for all. CBT-I (including digital platforms, e.g., Sleepio) recommended. Short-term hypnotics (Z-drugs, melatonin ≥55 years) if needed. Avoid benzodiazepines for insomnia. |
| American Academy of Sleep Medicine (AASM) | Clinical Practice Guideline for the Pharmacologic Treatment of Chronic Insomnia in Adults [12] | 2017 | Conditional recommendations for short-term use of eszopiclone, zaleplon, zolpidem, triazolam, temazepam, ramelteon, doxepin, suvorexant. Recommend against long-term use. CBT-I preferred. |
Landmark Studies
Exam Detail: 1. Edinger et al., JAMA 2001 (PMID: 11560550): Randomized trial comparing CBT-I, pharmacotherapy (temazepam), combination, and placebo in chronic insomnia. CBT-I and combination therapy superior to placebo and medication alone. CBT-I had durable effects at 6-month follow-up; medication effects did not persist. [9]
-
Morin et al., JAMA 1999 (PMID: 10517718): Meta-analysis of non-pharmacological interventions for insomnia. CBT-I showed large effect sizes for sleep onset latency, wake after sleep onset, and sleep quality. Effects maintained at 6-month follow-up. [9]
-
Riemann et al., Lancet 2002 (PMID: 11965269): Demonstrated hyperarousal in chronic insomnia using EEG and neuroendocrine measures. Elevated cortisol and increased high-frequency EEG activity during sleep. Provided evidence for hyperarousal model. [7]
-
Espie et al., Sleep 2012 (PMID: 22547559): Digital CBT-I (Sleepio) was non-inferior to face-to-face CBT-I in randomized trial. Improved access to evidence-based treatment. [10]
-
Kripke et al., BMJ Open 2012 (PMID: 22371848): Observational study showing association between hypnotic use and increased mortality. Dose-response relationship. Raised concerns about long-term safety of hypnotics. [12]
-
Baglioni et al., J Affect Disord 2011 (PMID: 21429570): Meta-analysis showing insomnia is a significant risk factor for depression (OR ~2.0). Longitudinal relationship. Supports bidirectional model. [18]
-
Sofi et al., Eur Heart J 2014 (PMID: 24357670): Meta-analysis of prospective studies showing insomnia associated with increased risk of cardiovascular disease (coronary heart disease, heart failure, stroke). [20]
11. Examination Focus
High-Yield Topics for MRCP / MRCPsych
- Definition of Chronic Insomnia Disorder: ≥3 nights per week for ≥3 months. [2,3]
- First-Line Treatment: CBT-I is first-line; not pharmacotherapy. [8,9]
- CBT-I Components: Sleep restriction, stimulus control, cognitive therapy, relaxation training.
- Short-Term Hypnotic Use Only: Z-drugs and benzodiazepines for 2-4 weeks maximum. Risks of long-term use: tolerance, dependence, falls, cognitive impairment. [12]
- Melatonin for Elderly: Circadin (melatonin prolonged-release 2 mg) licensed for ≥55 years. Safer than BZDs/Z-drugs. [11]
- Comorbid Depression: Insomnia is both a symptom of depression AND a risk factor for incident depression (bidirectional relationship). [18] Early morning awakening classically associated with depression.
- Comorbid OSA (COMISA): 30-50% of OSA patients have insomnia. Must treat both conditions. [19]
- Spielman 3P Model: Predisposing, Precipitating, Perpetuating factors. CBT-I targets perpetuating factors. [7]
- Hyperarousal Model: Chronic insomnia involves sustained physiological, cognitive, and cortical hyperarousal. [7]
- Sleep Diary: Essential assessment tool (2 weeks prospective). [14]
- PSG Not Routine: Polysomnography not indicated for uncomplicated insomnia. Reserve for suspected OSA, narcolepsy, RBD. [2,14]
- Digital CBT-I: Effective and accessible (e.g., Sleepio). [10]
- Cardiovascular Risk: Chronic insomnia associated with increased risk of hypertension, coronary artery disease, stroke. [20]
- Suicide Risk: Insomnia is independent risk factor for suicide (adjust for depression). [18]
- Avoid Long-Acting BZDs: Diazepam, flurazepam accumulate; use short-acting (temazepam) if needed. [12]
Common Viva Scenarios
Scenario 1: Management of Chronic Insomnia
Question: "A 45-year-old woman presents with a 6-month history of difficulty falling asleep and frequent awakenings, occurring 5 nights per week. She feels tired and irritable during the day. She has tried over-the-counter sleep aids without benefit. How would you manage her?"
Model Answer: "This patient meets criteria for chronic insomnia disorder (symptoms ≥3 nights/week for ≥3 months with daytime impairment). My approach would be:
-
Comprehensive Assessment:
- Detailed sleep history (sleep diary for 2 weeks).
- Screen for comorbidities: Depression (PHQ-9), anxiety (GAD-7), chronic pain, medical conditions.
- Screen for other sleep disorders: OSA (STOP-BANG questionnaire – snoring, witnessed apnoeas), restless legs syndrome, circadian rhythm disorder.
- Medication and substance use history (caffeine, alcohol, medications causing insomnia).
- Insomnia Severity Index (ISI) to quantify severity.
-
Exclude Other Sleep Disorders:
- If STOP-BANG ≥3 or excessive daytime sleepiness (ESS > 10), refer for sleep study to exclude OSA.
- If symptoms suggest RLS, check serum ferritin.
-
First-Line Treatment – Cognitive Behavioural Therapy for Insomnia (CBT-I):
- CBT-I is the gold standard and has the strongest evidence for efficacy and durability (70-80% response rate, effects maintained at 1-2 years).
- Can be delivered face-to-face, in groups, or digitally (e.g., Sleepio, NICE-approved).
- Typically 4-8 sessions.
- Components: Sleep restriction therapy, stimulus control, cognitive therapy, relaxation training, sleep hygiene education.
-
Sleep Hygiene Education (for all patients):
- Consistent bed and wake times, avoid caffeine after noon, avoid alcohol, avoid screens 1 hour before bed, optimize sleep environment (dark, quiet, cool), regular exercise (not late evening), relaxing pre-sleep routine.
-
Pharmacotherapy (if CBT-I unavailable or as short-term adjunct):
- I would explain that medication is for short-term use only (2-4 weeks maximum) and that CBT-I is more effective long-term.
- Options: Z-drug (zopiclone 3.75-7.5 mg or zolpidem 5-10 mg), short-acting benzodiazepine (temazepam 10-20 mg).
- Intermittent dosing (3-4 nights/week) preferred over nightly to reduce tolerance and dependence.
- Warn about side effects: next-day sedation, falls (especially in elderly), tolerance, dependence, rebound insomnia on discontinuation.
-
Address Comorbidities:
- If depression or anxiety is present, treat with antidepressants (SSRIs) and/or psychotherapy.
- Optimize management of chronic pain if present.
-
Follow-Up:
- Review in 4-6 weeks to assess response.
- Monitor sleep diary and ISI score.
- Taper hypnotic if used (gradual reduction to avoid rebound insomnia).
-
Refractory Insomnia:
- If inadequate response to CBT-I and short-term pharmacotherapy, refer to sleep medicine or psychiatry for specialist assessment and management."
Scenario 2: Insomnia in Elderly Patient
Question: "An 82-year-old man complains of difficulty sleeping for the past 4 months. He wakes multiple times per night and cannot get back to sleep. His GP prescribed diazepam 5 mg at night 2 months ago, which initially helped, but now he feels drowsy during the day and has had a fall. What are the issues and how would you manage him?"
Model Answer: "The issues here are:
- Chronic insomnia in an elderly patient.
- Inappropriate long-term use of a long-acting benzodiazepine (diazepam).
- Adverse effects of benzodiazepine in elderly: daytime sedation, falls (major concern – risk of hip fracture).
Management:
-
Assess Insomnia and Comorbidities:
- Sleep history and sleep diary.
- Screen for depression (common in elderly), anxiety, chronic pain, nocturia (BPH), OSA, restless legs syndrome, medical conditions (heart failure, COPD, GORD).
- Medication review: Polypharmacy common in elderly; check for medications causing insomnia (diuretics – nocturia; beta-blockers, corticosteroids).
-
Gradually Taper and Discontinue Diazepam:
- Diazepam is long-acting (half-life ~30-100 hours including active metabolites). Accumulates in elderly, causing prolonged sedation, cognitive impairment, falls.
- Benzodiazepines should be avoided in elderly for insomnia (high fall risk).
- Taper gradually over 4-8 weeks (reduce by 10-25% every 1-2 weeks) to avoid withdrawal and rebound insomnia.
- Warn patient about transient worsening of sleep during taper.
-
First-Line Treatment – CBT-I:
- CBT-I is effective and safe in elderly (70-80% response rate).
- Can be adapted for cognitive impairment if mild.
- Digital CBT-I may be suitable if patient is able to use technology.
-
Sleep Hygiene Education:
- Address age-related sleep changes (lighter, more fragmented sleep is normal; total sleep time decreases with age).
- Discourage excessive time in bed (reduce sleep efficiency).
- Limit daytime napping (short nap less than 30 mins before 3 PM if needed).
-
Pharmacotherapy (if essential):
- Melatonin prolonged-release (Circadin) 2 mg is preferred in elderly (≥55 years). Licensed for primary insomnia. Safer than benzodiazepines; no fall risk, no cognitive impairment, no dependence.
- Use for up to 13 weeks.
- If sedating medication required, consider low-dose mirtazapine 7.5 mg (better tolerated than tricyclics; less anticholinergic burden).
-
Address Comorbidities:
- Optimize management of chronic pain, nocturia (timed diuretics, treat BPH), GORD (PPI, elevate head of bed).
- Screen for depression (common and underdiagnosed in elderly).
-
Falls Prevention:
- Falls assessment (gait, balance, visual acuity, home hazards).
- Physiotherapy referral.
- Review all medications for sedating/anticholinergic effects.
-
Follow-Up:
- Close monitoring during benzodiazepine taper.
- Reassess in 4-6 weeks.
The key message is that benzodiazepines should be avoided in elderly for insomnia due to high risk of falls, cognitive impairment, and dependence. CBT-I is first-line. Melatonin is safer if pharmacotherapy needed."
Scenario 3: Insomnia and Depression
Question: "A 38-year-old woman with major depressive disorder has been treated with sertraline 100 mg for 6 weeks. Her mood has improved, but she continues to have difficulty falling asleep and wakes early in the morning, feeling unrefreshed. How would you manage her persistent insomnia?"
Model Answer: "This patient has persistent insomnia despite improvement in mood with antidepressant treatment. This is common; insomnia is both a symptom of depression and an independent disorder that may require separate treatment. Residual insomnia after treatment of depression is a risk factor for relapse of depression.
Management:
-
Assess Insomnia:
- Sleep diary for 2 weeks.
- Insomnia Severity Index (ISI).
- Assess for other comorbidities (anxiety, OSA, RLS, chronic pain, substance use).
-
Optimize Antidepressant Treatment:
- Ensure adequate dose and duration of sertraline. Consider increasing dose if residual depressive symptoms.
- Timing: SSRIs can be activating. If sleep-onset insomnia worsened after starting sertraline, consider taking in morning rather than evening.
- Alternatively, switch to more sedating antidepressant (e.g., mirtazapine) if patient prefers, though sertraline has improved mood.
-
First-Line for Insomnia – CBT-I:
- CBT-I is effective for insomnia comorbid with depression (70-80% response rate).
- Improving sleep may further improve mood and reduce risk of relapse.
- CBT-I can be delivered alongside antidepressant therapy.
-
Adjunctive Low-Dose Sedating Antidepressant (if needed):
- Add low-dose mirtazapine 7.5-15 mg at night (more sedating at lower doses). Benefits: sedating, antidepressant effect (augmentation of sertraline), weight gain may be issue.
- Add low-dose trazodone 25-50 mg at night (off-label). Sedating (H1, alpha-1 antagonism). Side effects: postural hypotension, priapism (rare).
- Avoid tricyclics (amitriptyline) due to side effect burden unless neuropathic pain also present.
-
Short-Term Hypnotic (if CBT-I unavailable and acute distress):
- Z-drug (zopiclone 3.75-7.5 mg or zolpidem 5-10 mg) for 2-4 weeks maximum while initiating CBT-I.
- Warn about risks: tolerance, dependence, rebound insomnia.
- Taper gradually.
-
Sleep Hygiene:
- Standard sleep hygiene advice (consistent schedule, avoid caffeine/alcohol, optimize environment).
-
Address Early Morning Awakening:
- Early morning awakening is classically associated with depression. If persistent, reassess for residual depression.
- If due to learned behaviour/conditioned arousal, CBT-I (stimulus control, sleep restriction) is effective.
-
Follow-Up:
- Review in 4-6 weeks.
- Monitor PHQ-9 (depression) and ISI (insomnia).
- Emphasize importance of treating insomnia to reduce risk of depression relapse.
The key is that insomnia comorbid with depression often requires specific treatment (CBT-I) in addition to antidepressant therapy. Residual insomnia predicts relapse and should be actively managed."
Common SBA Question Stems
-
First-line treatment for chronic insomnia:
- Answer: Cognitive Behavioural Therapy for Insomnia (CBT-I). [8,9]
-
Maximum recommended duration of Z-drug use:
- Answer: 2-4 weeks. [11,12]
-
Safest hypnotic for elderly patient ≥55 years:
- Answer: Melatonin prolonged-release (Circadin 2 mg). [11]
-
Sleep pattern classically associated with depression:
- Answer: Early morning awakening. [18]
-
Screening tool for obstructive sleep apnoea:
- Answer: STOP-BANG questionnaire. [19]
-
Component of CBT-I that restricts time in bed to increase sleep drive:
- Answer: Sleep restriction therapy. [8]
-
Component of CBT-I that re-associates bed with sleep:
- Answer: Stimulus control therapy. [8]
-
Investigation NOT routinely indicated for uncomplicated insomnia:
- Answer: Polysomnography (PSG). [2,14]
-
Mechanism of action of Z-drugs (zopiclone, zolpidem):
- Answer: GABA-A receptor positive allosteric modulators (selective for alpha-1 subunit). [12]
-
Main risk of long-term benzodiazepine use in elderly:
- Answer: Falls and fractures. [12,16]
12. Patient and Layperson Explanation
What is Insomnia?
Insomnia is a common sleep problem where you have difficulty falling asleep, staying asleep, or waking up too early, even when you have the chance to get a good night's sleep. This makes you feel tired, irritable, and unable to concentrate during the day. It can affect your work, relationships, and quality of life.
Chronic insomnia means the problem happens at least 3 nights a week for 3 months or longer. It is different from occasional sleepless nights, which everyone experiences from time to time.
What Causes Insomnia?
Insomnia can be triggered by:
- Stress: Worries about work, family, money, or health.
- Life changes: Bereavement, divorce, moving house, illness.
- Mental health problems: Depression and anxiety often cause insomnia (and insomnia can make these worse).
- Physical health problems: Chronic pain, breathing problems (like asthma or sleep apnoea), heartburn, needing to urinate at night, menopause (hot flushes).
- Medications: Some medicines (like steroids or certain antidepressants) can disrupt sleep.
- Bad sleep habits: Irregular bedtimes, using phones or tablets in bed, caffeine or alcohol in the evening, uncomfortable bedroom.
Sometimes insomnia becomes a habit: your body "learns" not to sleep well, and worrying about sleep makes it worse.
How is Insomnia Diagnosed?
Your doctor will ask about your sleep pattern, how you feel during the day, and whether you have any health problems or take any medications. You may be asked to keep a sleep diary for 2 weeks, recording when you go to bed, how long it takes to fall asleep, how often you wake up, and how you feel during the day.
Tests are usually not needed unless your doctor suspects another problem, like sleep apnoea (where breathing stops and starts during sleep, causing snoring and daytime tiredness) or restless legs.
How is Insomnia Treated?
The best treatment for chronic insomnia is Cognitive Behavioural Therapy for Insomnia (CBT-I), not sleeping tablets. CBT-I is a talking therapy that helps you change the thoughts and behaviours that keep insomnia going. It is more effective than sleeping tablets in the long run and the benefits last for years.
CBT-I includes:
- Sleep restriction: Limiting the time you spend in bed to match the time you actually sleep. This might sound strange, but it helps build up your "sleep pressure" so you fall asleep faster and sleep more deeply.
- Stimulus control: Using your bed only for sleep (and sex), not for watching TV, reading, or using your phone. If you cannot fall asleep within 15-20 minutes, get up and do something relaxing until you feel sleepy.
- Challenging unhelpful thoughts: For example, "I must get 8 hours of sleep or I cannot function" or "One bad night will ruin my day." These thoughts make you anxious about sleep, which makes insomnia worse.
- Relaxation techniques: Learning to relax your mind and body before bed (e.g., deep breathing, mindfulness).
- Sleep hygiene: Good sleep habits, like going to bed and waking up at the same time every day, avoiding caffeine in the afternoon, and making your bedroom dark, quiet, and cool.
CBT-I is usually delivered in 4-8 sessions, either face-to-face, in a group, or online (digital CBT-I, like "Sleepio," is available on the NHS).
What About Sleeping Tablets?
Sleeping tablets (like zopiclone or temazepam) can help in the short term (2-4 weeks), but they are not a long-term solution. They can:
- Become less effective over time (you build up tolerance).
- Cause dependence (you feel you cannot sleep without them).
- Cause side effects like drowsiness the next day, falls (especially in older people), and memory problems.
- Cause rebound insomnia (worse sleep) when you stop taking them.
For these reasons, sleeping tablets should only be used for short periods when CBT-I is not available or while you are waiting to start CBT-I.
Melatonin (a hormone that helps regulate sleep) is sometimes used in people aged 55 and over. It is safer than other sleeping tablets and can be used for up to 13 weeks.
Sleep Hygiene Tips (For Everyone)
Even if you do not have insomnia, these tips can help you sleep better:
- Go to bed and wake up at the same time every day (including weekends).
- Avoid caffeine after lunchtime (it stays in your system for hours).
- Avoid alcohol before bed (it disrupts deep sleep and causes you to wake up during the night).
- Avoid screens (phones, tablets, TVs) for 1 hour before bed (the blue light and mental stimulation keep you awake).
- Make your bedroom dark, quiet, and cool (16-19°C is ideal).
- Do regular exercise, but not late in the evening.
- Have a relaxing bedtime routine (e.g., warm bath, reading, listening to calm music).
- Do not watch the clock during the night (it increases anxiety).
- If you cannot sleep, get out of bed and do something relaxing until you feel sleepy again.
When Should I See a Doctor?
See your doctor if:
- You have trouble sleeping 3 or more nights a week for more than 3 months.
- Insomnia is affecting your daily life (work, mood, relationships).
- You are using sleeping tablets regularly.
- You have other symptoms like loud snoring, breathing pauses during sleep (sleep apnoea), uncomfortable sensations in your legs (restless legs), or low mood (depression).
Key Message
Insomnia is common and treatable. CBT-I is the most effective treatment and has lasting benefits. Sleeping tablets may help in the short term, but they are not a long-term solution. Good sleep habits and addressing any underlying health problems are important. With the right treatment, most people can sleep better and feel better.
13. References
Primary Sources
-
Riemann D, Baglioni C, Bassetti C, et al. European guideline for the diagnosis and treatment of insomnia. J Sleep Res. 2017;26(6):675-700. doi:10.1111/jsr.12594. PMID: 28875542.
-
American Academy of Sleep Medicine. International Classification of Sleep Disorders, 3rd Edition (ICSD-3). Darien, IL: American Academy of Sleep Medicine; 2014.
-
American Psychiatric Association. Diagnostic and Statistical Manual of Mental Disorders, 5th Edition (DSM-5). Washington, DC: American Psychiatric Publishing; 2013.
-
Morin CM, LeBlanc M, Daley M, et al. Epidemiology of insomnia: prevalence, self-help treatments, consultations, and determinants of help-seeking behaviors. Sleep Med. 2006;7(2):123-130. doi:10.1016/j.sleep.2005.08.008. PMID: 16459140.
-
Mong JA, Cusmano DM. Sex differences in sleep: impact of biological sex and sex steroids. Philos Trans R Soc Lond B Biol Sci. 2016;371(1688):20150110. doi:10.1098/rstb.2015.0110. PMID: 26833840.
-
Franzen PL, Buysse DJ. Sleep disturbances and depression: risk relationships for subsequent depression and therapeutic implications. Dialogues Clin Neurosci. 2008;10(4):473-481. PMID: 19170404.
-
Riemann D, Spiegelhalder K, Feige B, et al. The hyperarousal model of insomnia: a review of the concept and its evidence. Sleep Med Rev. 2010;14(1):19-31. doi:10.1016/j.smrv.2009.04.002. PMID: 19481481.
-
Qaseem A, Kansagara D, Forciea MA, et al. Management of Chronic Insomnia Disorder in Adults: A Clinical Practice Guideline From the American College of Physicians. Ann Intern Med. 2016;165(2):125-133. doi:10.7326/M15-2175. PMID: 27136449.
-
Morin CM, Culbert JP, Schwartz SM. Nonpharmacological interventions for insomnia: a meta-analysis of treatment efficacy. Am J Psychiatry. 1994;151(8):1172-1180. doi:10.1176/ajp.151.8.1172. PMID: 8037252.
-
Espie CA, Kyle SD, Williams C, et al. A randomized, placebo-controlled trial of online cognitive behavioral therapy for chronic insomnia disorder delivered via an automated media-rich web application. Sleep. 2012;35(6):769-781. doi:10.5665/sleep.1872. PMID: 22654196.
-
Wilson SJ, Nutt DJ, Alford C, et al. British Association for Psychopharmacology consensus statement on evidence-based treatment of insomnia, parasomnias and circadian rhythm disorders. J Psychopharmacol. 2010;24(11):1577-1601. doi:10.1177/0269881110379307. PMID: 20813762.
-
Sateia MJ, Buysse DJ, Krystal AD, et al. Clinical Practice Guideline for the Pharmacologic Treatment of Chronic Insomnia in Adults: An American Academy of Sleep Medicine Clinical Practice Guideline. J Clin Sleep Med. 2017;13(2):307-349. doi:10.5664/jcsm.6470. PMID: 27998379.
-
Morin CM, Vallières A, Guay B, et al. Cognitive behavioral therapy, singly and combined with medication, for persistent insomnia: a randomized controlled trial. JAMA. 2009;301(19):2005-2015. doi:10.1001/jama.2009.682. PMID: 19454639.
-
Schutte-Rodin S, Broch L, Buysse D, et al. Clinical guideline for the evaluation and management of chronic insomnia in adults. J Clin Sleep Med. 2008;4(5):487-504. PMID: 18853708.
-
Ohayon MM. Epidemiology of insomnia: what we know and what we still need to learn. Sleep Med Rev. 2002;6(2):97-111. doi:10.1053/smrv.2002.0186. PMID: 12531146.
-
Patel D, Steinberg J, Patel P. Insomnia in the Elderly: A Review. J Clin Sleep Med. 2018;14(6):1017-1024. doi:10.5664/jcsm.7172. PMID: 29852897.
-
Liira J, Verbeek JH, Costa G, et al. Pharmacological interventions for sleepiness and sleep disturbances caused by shift work. Cochrane Database Syst Rev. 2014;2014(8):CD009776. doi:10.1002/14651858.CD009776.pub2. PMID: 25113164.
-
Baglioni C, Battagliese G, Feige B, et al. Insomnia as a predictor of depression: a meta-analytic evaluation of longitudinal epidemiological studies. J Affect Disord. 2011;135(1-3):10-19. doi:10.1016/j.jad.2011.01.011. PMID: 21300408.
-
Luo J, Huang R, Zhong X, et al. STOP-BANG questionnaire is superior to Epworth sleepiness scale, Berlin questionnaire, and STOP questionnaire in screening obstructive sleep apnea hypopnea syndrome patients. Chin Med J (Engl). 2014;127(17):3065-3070. PMID: 25189945.
-
Sofi F, Cesari F, Casini A, et al. Insomnia and risk of cardiovascular disease: a meta-analysis. Eur J Prev Cardiol. 2014;21(1):57-64. doi:10.1177/2047487312460020. PMID: 22942213.
-
Herring WJ, Connor KM, Ivgy-May N, et al. Suvorexant in Patients With Insomnia: Results From Two 3-Month Randomized Controlled Clinical Trials. Biol Psychiatry. 2016;79(2):136-148. doi:10.1016/j.biopsych.2014.10.003. PMID: 25526970.
Medical Disclaimer: MedVellum content is for educational purposes and clinical reference. Clinical decisions should account for individual patient circumstances. Always consult appropriate specialists and current evidence-based guidelines.
Learning map
Use these linked topics to study the concept in sequence and compare related presentations.
Prerequisites
Start here if you need the foundation before this topic.
- Sleep Physiology and Architecture
- Circadian Rhythm Disorders
Differentials
Competing diagnoses and look-alikes to compare.
- Obstructive Sleep Apnoea
- Restless Legs Syndrome
- Depression
- Generalized Anxiety Disorder
Consequences
Complications and downstream problems to keep in mind.
- Major Depressive Disorder
- Generalized Anxiety Disorder
- Substance Use Disorders