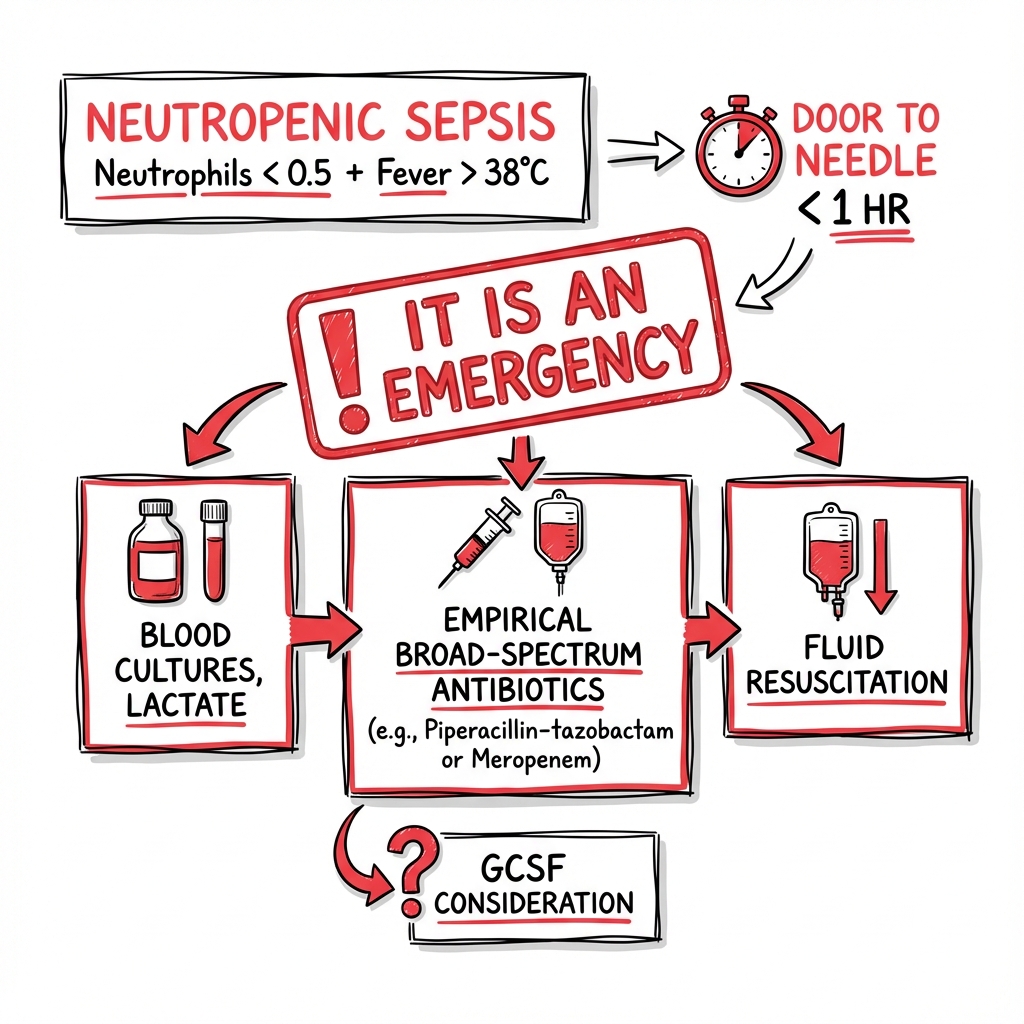
Neutropenic Sepsis
Neutropenic Sepsis (Febrile Neutropenia, FN) is a life-threatening oncological emergency defined by fever in the presenc... MRCP exam preparation.
What matters first
Neutropenic Sepsis (Febrile Neutropenia, FN) is a life-threatening oncological emergency defined by fever in the presenc... MRCP exam preparation.
Systolic BP less than 90 mmHg (Septic Shock)
6 Jan 2026
Generated educational material; verify before clinical use.
Visible references section
See the concept before reading it
Study the key anatomy, imaging, and decision pathways as full teaching plates.
Clinical board
A visual summary of the highest-yield teaching signals on this page.
Urgent signals
Safety-critical features pulled from the topic metadata.
- Systolic BP less than 90 mmHg (Septic Shock)
- Ecthyma gangrenosum (Black necrotic skin lesions - Pseudomonas)
- RLQ pain and distension (Typhlitis/Neutropenic Enterocolitis)
- New-onset hypoxia or 'Halo sign' on CT (Invasive Aspergillosis)
Exam focus
Current exam surfaces linked to this topic.
- MRCP
Linked comparisons
Differentials and adjacent topics worth opening next.
- Tumour Lysis Syndrome
- Graft Versus Host Disease
Content status and exam context
This page is AI-generated educational content. It may contain errors or omissions and is not a substitute for current guidelines, local protocols, senior clinical judgement, or professional medical advice.
MedVellum does not claim an individual clinician reviewer, board certification, or professional credential for this page unless a future version names a real, verifiable reviewer.
Clinical explanation and evidence
Neutropenic Sepsis (Adult)
1. Clinical Overview
Neutropenic Sepsis (Febrile Neutropenia, FN) is a life-threatening oncological emergency defined by fever in the presence of severe neutropenia (absolute neutrophil count less than 0.5 × 10^9/L). It represents the most common cause of treatment-related mortality in patients receiving myelosuppressive chemotherapy, accounting for 5-11% of all hospitalizations in cancer patients. [1,2]
Defining Characteristics
The catastrophic nature of neutropenic sepsis derives from three cardinal features:
-
Immunological Paralysis: The absence of neutrophils eliminates the host's primary defense against bacterial and fungal pathogens. Classic inflammatory signs (pus formation, abscess, lobar consolidation on chest radiograph) are frequently absent, making fever the sole clinical indicator of life-threatening infection.
-
Time-Critical Mortality: Survival is inversely proportional to "Door-to-Antibiotic" time. Every hour of delay in administering empirical broad-spectrum antibiotics in high-risk patients increases mortality by 18-20%. [3] Patients progressing to septic shock have a mortality rate exceeding 40%, compared to 1-5% in hemodynamically stable cases.
-
Microbial Shift: Historical dominance by Gram-negative organisms (particularly Pseudomonas aeruginosa) has shifted toward Gram-positive bacteria (60-70% of isolates), largely due to the widespread use of indwelling central venous catheters and fluoroquinolone prophylaxis. [4,5]
Contemporary Management Paradigm
The 2024 ASCO/IDSA guideline framework emphasizes:
- Immediate empirical antipseudomonal beta-lactam therapy within 60 minutes of presentation
- Risk stratification using the MASCC score to identify low-risk candidates for outpatient oral therapy
- Early escalation to empirical antifungal coverage (day 4-7) in persistent fever
- Judicious G-CSF use in high-risk subgroups (age >65, profound neutropenia, pneumonia, septic shock)
- De-escalation protocols based on clinical response and culture data [6,7]
2. Epidemiology
Incidence and Burden
Neutropenic sepsis complicates 10-50% of solid tumor chemotherapy regimens and occurs in >80% of patients with hematological malignancies undergoing intensive induction chemotherapy. [8] The overall incidence is increasing due to:
- More aggressive chemotherapy protocols
- Expanding use of dose-dense regimens in solid tumors
- Rising numbers of hematopoietic stem cell transplantations
- Increasing population of elderly cancer patients (age >65)
The Nadir Window
Temporal Profile: Most episodes occur 7-14 days post-chemotherapy, coinciding with the "nadir" of bone marrow suppression. This timing reflects:
- Neutrophil half-life of 6-8 hours in circulation
- Delayed recovery of bone marrow progenitors (typically 14-21 days)
- Overlapping gastrointestinal mucositis (peak days 5-10)
High-Risk Chemotherapy Regimens (FN risk >20%):
- Docetaxel-based combinations (breast cancer)
- FOLFOX (colorectal cancer)
- Cisplatin + etoposide (lung cancer)
- R-CHOP (lymphoma)
- Induction regimens for acute leukemia (cytarabine + anthracycline)
Mortality Stratification
| Clinical Scenario | Mortality Rate | Key Determinants |
|---|---|---|
| Low-Risk FN (MASCC ≥21) | 1-3% | Solid tumor, ANC nadir brief (less than 7 days), outpatient onset |
| High-Risk FN (MASCC less than 21) | 10-15% | Hematological malignancy, profound neutropenia (ANC less than 0.1), inpatient onset |
| Septic Shock | 40-60% | Persistent hypotension, multi-organ dysfunction |
| Invasive Fungal Infection | 30-50% | Prolonged neutropenia (>10 days), GVHD, corticosteroids |
The Microbial Shift
| Era | Dominant Organisms | Drivers |
|---|---|---|
| Pre-1990 | Gram-negative (70%): Pseudomonas, E. coli, Klebsiella | No prophylaxis, minimal central lines |
| 1990-2010 | Transition phase: 50/50 Gram-positive/Gram-negative | Fluoroquinolone prophylaxis, CVC use |
| 2010-Present | Gram-positive (60-70%): CoNS, Viridans strep, Enterococcus | Universal CVC, mucositis, FQ resistance |
| Emerging Threat | MDR Gram-negatives: ESBL-producing E. coli, Klebsiella; Carbapenem-resistant Pseudomonas | Antibiotic pressure, global resistance trends |
Fungal infections (primarily Candida and Aspergillus species) account for 5-10% of microbiologically documented infections but disproportionately contribute to mortality in cases of prolonged neutropenia (>10 days). [9,10]
3. Aetiology and Pathophysiology
Etiology: The Triad of Risk
Neutropenic sepsis arises from the convergence of three pathophysiological insults:
1. Chemotherapy-Induced Myelosuppression
Cytotoxic chemotherapy agents non-selectively target rapidly dividing cells, including hematopoietic stem cells in the bone marrow. The brief circulating half-life of neutrophils (6-8 hours) ensures rapid depletion following cessation of production.
High-Risk Agents:
- Alkylating agents (cyclophosphamide, ifosfamide)
- Anthracyclines (doxorubicin, daunorubicin)
- Antimetabolites (cytarabine, methotrexate)
- Taxanes (docetaxel, paclitaxel)
- Platinum compounds (cisplatin, carboplatin)
Duration and Depth: The "depth" (nadir ANC) and "duration" (days with ANC less than 0.5) are the primary determinants of infection risk. Profound neutropenia (ANC less than 0.1 × 10^9/L) sustained for >7 days confers a near-100% risk of serious bacterial or fungal infection. [11]
2. Mucosal Barrier Disruption
Chemotherapy also damages rapidly dividing enterocytes lining the gastrointestinal tract, leading to mucositis. This creates:
- Physical barrier loss: Denuded mucosa allows direct translocation of luminal bacteria
- Loss of secretory IgA: Further compromises mucosal defense
- Dysbiosis: Antibiotic pressure and chemotherapy itself alter the protective commensal microbiome
Grade 3-4 oral mucositis (confluent ulceration, inability to eat) is an independent predictor of Viridans group streptococcal bacteremia and acute respiratory distress syndrome (ARDS). [12]
3. Indwelling Central Venous Catheters
Central venous catheters (CVCs) provide a direct conduit for skin commensals (Staphylococcus epidermidis, Staphylococcus aureus) to enter the bloodstream. Biofilm formation on catheter surfaces protects bacteria from antibiotics and immune clearance, contributing to persistent bacteremia.
Molecular Pathophysiology: The 7-Step Cascade
Step 1: Chemotherapy Myelosuppression
Cytotoxic agents disrupt the mitotic activity of hematopoietic stem cells in the bone marrow niche. Apoptosis of granulocyte precursors and brief neutrophil half-life lead to rapid depletion.
Step 2: Mucosal Barrier Breach
Chemotherapy induces apoptosis in enterocytes, resulting in mucosal ulceration and loss of tight junction integrity. The physical barrier between the microbiome (10^14 organisms) and the bloodstream is breached.
Step 3: Pathobiont Translocation
Commensal bacteria (Escherichia coli, Klebsiella pneumoniae, Pseudomonas aeruginosa) and fungi (Candida albicans) translocate across the damaged mucosa into the lamina propria and mesenteric lymphatics, gaining access to the portal and systemic circulation.
Step 4: Impaired Innate Sensing
Tissue-resident macrophages detect pathogen-associated molecular patterns (PAMPs) via Toll-like receptors (TLRs) and initiate cytokine release (TNF-α, IL-1β, IL-6). However, the CXCL8 (IL-8) chemokine gradient fails to recruit neutrophils because they are absent from circulation.
Step 5: Unchecked Microbial Proliferation
Without neutrophil-mediated phagocytosis and oxidative killing, bacterial doubling time proceeds unimpeded (~20-30 minutes for E. coli). High-grade bacteremia (10^5-10^7 CFU/mL) develops rapidly, overwhelming residual immune defenses.
Step 6: Dysregulated Cytokine Storm
Systemic release of pro-inflammatory cytokines (TNF-α, IL-1β, IL-6) induces fever and activates the coagulation cascade. Endothelial activation, glycocalyx shedding, and capillary leak lead to distributive shock. Compensatory anti-inflammatory mechanisms (IL-10, cortisol) are impaired, resulting in immune paralysis.
Step 7: Multi-Organ Dysfunction
Microvascular thrombosis, mitochondrial dysfunction, and cellular dysoxia culminate in acute kidney injury, acute respiratory distress syndrome, hepatic dysfunction, and coagulopathy. Death occurs from refractory shock and multi-organ failure. [13,14,15]
The "Cryptic Infection" Phenomenon
In neutropenic patients, classic signs of localized infection are absent:
- No purulent sputum in pneumonia (neutrophils produce pus)
- No lobar consolidation on chest radiograph (consolidation is inflammatory exudate + neutrophils)
- No abscess formation (abscesses are walled-off collections of neutrophils and debris)
- No pyuria in urinary tract infection
This "cryptic infection" paradox delays diagnosis and necessitates reliance on fever as the sole sentinel clinical sign.
4. Clinical Presentation
Fever Definition
Fever in Neutropenic Sepsis (IDSA/ASCO criteria):
- Single oral temperature ≥38.3°C (101°F)
- OR sustained temperature ≥38.0°C (100.4°F) for >1 hour
Critical Exception: 10-15% of severely neutropenic patients with documented infection are normothermic or hypothermic. Hypothermia (less than 36°C) is a poor prognostic indicator associated with shock and high mortality. [16]
Clinical Assessment: The "Fever-Plus" Approach
Cardinal Symptom: Fever
In many cases, fever is the only manifestation. Comprehensive clinical assessment must actively seek occult sources.
Site-Specific Presentations
1. Respiratory Tract (30-40% of documented infections)
- Symptoms: Cough (often non-productive), dyspnea, pleuritic chest pain
- Signs: Tachypnea, hypoxia (SpO2 less than 92%), diminished breath sounds
- Cryptic Feature: Absence of lobar consolidation on CXR due to lack of neutrophil-mediated inflammatory response
- Key Investigation: High-resolution CT chest reveals ground-glass opacities, nodules, or "halo sign" (Aspergillus) not visible on plain radiograph [17]
2. Gastrointestinal Tract (15-20%)
- Typhlitis (Neutropenic Enterocolitis): RLQ pain, distension, diarrhea (often bloody)
- Involves cecum and ascending colon
- "CT findings: Bowel wall thickening (>4 mm), pericolic stranding, pneumatosis"
- "Organisms: Mixed enteric flora, Clostridium septicum"
- "Complications: Perforation, shock, 30-50% mortality [18]"
- Perianal Infection: Severe perianal pain, erythema, induration
- Avoid digital rectal examination (risk of bacteremia)
- MRI pelvis if abscess suspected (CT less sensitive)
3. Skin and Soft Tissue (10-15%)
- Ecthyma Gangrenosum: Painless, indurated, necrotic black-centered ulcers with erythematous halo
- Pathognomonic for Pseudomonas aeruginosa
- Represents direct vascular invasion with thrombosis and tissue necrosis
- Requires immediate anti-pseudomonal beta-lactam + aminoglycoside
- Catheter-site cellulitis: Erythema, warmth, purulent discharge at CVC insertion site
- "Organisms: Staphylococcus aureus, coagulase-negative staphylococci"
4. Central Nervous System (Rare, less than 5%)
- Symptoms: Headache, altered mental status, seizures, focal neurological deficits
- Organisms: Listeria monocytogenes, Cryptococcus neoformans, Aspergillus (cerebral abscess), HSV, VZV
- Investigation: CT head (to exclude raised ICP) → lumbar puncture (if safe)
- CSF in neutropenic meningitis: May have low or absent white cell count despite active infection
5. Urinary Tract (10-15%)
- Symptoms: Dysuria, frequency, urgency (often absent)
- Signs: Suprapubic tenderness
- Caveat: Pyuria may be absent (no neutrophils to produce white cells in urine)
- Organisms: E. coli, Klebsiella, Enterococcus, Candida
Red Flag Clinical Scenarios
| Red Flag | Implication | Immediate Action |
|---|---|---|
| Systolic BP less than 90 mmHg | Septic shock | Fluid resuscitation (30 mL/kg crystalloid), vasopressors (norepinephrine), ICU transfer |
| Ecthyma gangrenosum | Pseudomonas bacteremia | Anti-pseudomonal beta-lactam + aminoglycoside, surgical debridement |
| RLQ pain + distension | Typhlitis | NPO, NG decompression, surgical consultation, CT abdomen/pelvis, broad-spectrum antibiotics including anaerobic coverage |
| New hypoxia + nodules on CT | Invasive pulmonary aspergillosis | Voriconazole or liposomal amphotericin B, galactomannan/beta-D-glucan, bronchoscopy |
| Altered mental status | CNS infection or septic encephalopathy | CT head, LP (if no contraindication), empirical aciclovir + ceftriaxone + ampicillin |
| Perianal pain | Perianal abscess | Avoid DRE, MRI pelvis, surgical consultation |
| ANC less than 0.1 × 10^9/L | Profound neutropenia, high mortality | Consider G-CSF, ICU-level monitoring |
5. Investigations
Immediate Diagnostic Workup (Within 60 Minutes)
1. Complete Blood Count with Differential
Absolute Neutrophil Count (ANC) Calculation:
ANC = WBC × (% Neutrophils + % Bands)
Neutropenia Severity Classification:
- Mild: 1.0–1.5 × 10^9/L (low infection risk)
- Moderate: 0.5–1.0 × 10^9/L (moderate risk)
- Severe: less than 0.5 × 10^9/L (high risk, diagnostic threshold for FN)
- Profound: less than 0.1 × 10^9/L (very high risk, mortality >20%)
Duration of Neutropenia:
- Brief: less than 7 days (lower infection risk)
- Prolonged: ≥7 days (high risk of invasive fungal infection)
2. Blood Cultures
Standard Protocol:
- Two sets of blood cultures (aerobic and anaerobic bottles)
- One set from peripheral vein (aseptic venipuncture)
- One set from each lumen of central venous catheter (if present)
Rationale for CVC Cultures:
- Catheter-related bloodstream infection (CRBSI) suspected if CVC culture is positive ≥2 hours before peripheral culture (differential time to positivity)
- Allows identification of biofilm-associated organisms
Yield: Blood cultures are positive in only 20-30% of neutropenic sepsis cases. Absence of positive culture does not exclude serious infection. [19]
3. Serum Lactate
- Purpose: Marker of tissue hypoperfusion and anaerobic metabolism
- Interpretation:
- "Lactate less than 2 mmol/L: Normal"
- "Lactate 2-4 mmol/L: Mild hypoperfusion"
- "Lactate >4 mmol/L: Severe shock, poor prognosis"
- Prognostic Value: Lactate >4 mmol/L associated with 40-60% mortality in neutropenic septic shock [20]
4. Renal and Hepatic Function
- Urea, Creatinine, eGFR: Assess renal function (guides antibiotic dosing, identifies acute kidney injury)
- Liver Enzymes (ALT, AST, ALP, Bilirubin): Hepatic dysfunction may indicate hepatosplenic candidiasis or sepsis-induced cholestasis
5. Coagulation Profile
- PT, APTT, Fibrinogen, D-Dimer: Screen for disseminated intravascular coagulation (DIC)
- DIC Criteria: Thrombocytopenia, prolonged PT/APTT, hypofibrinogenemia, elevated D-dimer
6. C-Reactive Protein (CRP) and Procalcitonin (PCT)
- CRP: Elevated in bacterial infection, but non-specific
- Procalcitonin: More specific for bacterial infection; PCT >0.5 ng/mL suggests bacterial sepsis
- Limitation: Both may be blunted in profound neutropenia due to impaired inflammatory response [21]
Site-Directed Investigations
Respiratory Symptoms
1. Chest Radiograph (CXR):
- Limitation: Low sensitivity in neutropenic patients (absence of neutrophils prevents lobar consolidation)
- Findings: Often normal despite severe pneumonia; may show subtle interstitial infiltrates
2. High-Resolution CT Chest (HRCT):
- Indications: Persistent fever, respiratory symptoms, abnormal auscultation, hypoxia
- Key Findings:
- ""Halo Sign": Ground-glass opacity surrounding a nodule (early invasive aspergillosis)"
- ""Air-Crescent Sign": Crescent of air around a cavitating nodule (late aspergillosis, indicates neutrophil recovery)"
- "Ground-glass opacities: Pneumocystis jirovecii pneumonia (PJP), viral pneumonia"
- "Tree-in-bud pattern: Bacterial bronchopneumonia"
3. Sputum Culture:
- Often unobtainable (patients cannot produce sputum)
- Consider bronchoscopy with bronchoalveolar lavage (BAL) if diagnosis uncertain and patient stable
Urinary Symptoms
1. Urinalysis and Urine Culture:
- Caveat: Pyuria may be absent in neutropenic patients
- Organisms: E. coli, Klebsiella, Enterococcus, Candida
Gastrointestinal Symptoms
1. Stool Culture and Clostridium difficile Toxin:
- If diarrhea present (C. difficile common in chemotherapy patients)
2. CT Abdomen/Pelvis:
- Indications: Abdominal pain, RLQ tenderness, distension
- Typhlitis Findings: Cecal wall thickening (>4 mm), pericolic stranding, bowel wall edema, pneumatosis
Neurological Symptoms
1. CT Head (Non-Contrast):
- Exclude raised intracranial pressure, hemorrhage, mass lesion before lumbar puncture
2. Lumbar Puncture:
- Contraindications: Platelets less than 50 × 10^9/L (relative), raised ICP, focal neurology
- CSF Analysis: Cell count (may be low despite infection), protein, glucose, Gram stain, culture, cryptococcal antigen, HSV/VZV PCR
Fungal Diagnostic Markers
1. Serum Galactomannan
- Target: Aspergillus cell wall component
- Optical Density Index (ODI) ≥0.5: Positive (sensitivity 70%, specificity 90%)
- False Positives: Piperacillin-tazobactam, cross-reactivity with other fungi
- Use: Serial monitoring (twice weekly) in high-risk patients (prolonged neutropenia, GVHD)
2. Serum (1→3)-β-D-Glucan
- Target: Fungal cell wall component (Candida, Aspergillus, Pneumocystis)
- Cutoff: >80 pg/mL positive
- Sensitivity: 75-80% for invasive fungal infection
- False Positives: Hemodialysis, IV immunoglobulin, gauze exposure
3. Aspergillus PCR
- Emerging tool with high sensitivity; not yet widely available
Risk Stratification: MASCC Score
The Multinational Association for Supportive Care in Cancer (MASCC) Risk Index stratifies patients into low-risk (outpatient oral therapy candidates) vs. high-risk (mandatory inpatient IV therapy). [22]
| Clinical Feature | Points |
|---|---|
| Burden of illness: No or mild symptoms | 5 |
| Burden of illness: Moderate symptoms | 3 |
| No hypotension (SBP ≥90 mmHg) | 5 |
| No chronic obstructive pulmonary disease | 4 |
| Solid tumor or hematologic malignancy with no previous fungal infection | 4 |
| No dehydration requiring IV fluids | 3 |
| Outpatient status at onset of fever | 3 |
| Age less than 60 years | 2 |
Interpretation:
- MASCC Score ≥21: Low Risk (mortality less than 5%)
- Eligible for outpatient oral antibiotic therapy (if other low-risk criteria met)
- "Oral regimen: Ciprofloxacin 500-750 mg BD + Amoxicillin-clavulanate 625 mg TDS"
- MASCC Score less than 21: High Risk (mortality 10-40%)
- Mandatory inpatient admission
- IV empirical broad-spectrum antibiotics
- Close monitoring for clinical deterioration
Exclusion Criteria for Outpatient Management (regardless of MASCC score):
- Hemodynamic instability (hypotension, tachycardia)
- New-onset hypoxia or respiratory distress
- Altered mental status
- Severe mucositis (inability to tolerate oral intake)
- Uncontrolled pain or vomiting
- ANC less than 0.1 × 10^9/L (profound neutropenia)
- Expected prolonged neutropenia (>7 days)
6. Management
The 60-Minute Mandate
Guiding Principle: Empirical broad-spectrum antibiotics must be administered within 60 minutes of presentation. Every hour of delay increases mortality by 18-20% in high-risk patients. [3]
Step 1: Immediate Resuscitation and Stabilization
Airway, Breathing, Circulation
Oxygen:
- Target SpO2 >94% (or 88-92% in COPD)
- Escalate to non-invasive ventilation or intubation if respiratory failure
IV Fluid Resuscitation:
- Septic Shock Protocol: 30 mL/kg crystalloid bolus (Hartmann's or 0.9% saline) within first hour
- Reassess perfusion (lactate, urine output, capillary refill, mental status)
Vasopressors:
- If hypotension persists despite fluid resuscitation, initiate norepinephrine via central line
- Target mean arterial pressure (MAP) ≥65 mmHg
ICU Transfer Indications:
- Septic shock (persistent hypotension despite fluids)
- Respiratory failure requiring mechanical ventilation
- Multi-organ dysfunction
- Lactate >4 mmol/L
Step 2: Empirical Antibiotic Therapy
High-Risk Patients (MASCC less than 21, Inpatient)
First-Line Monotherapy (covers Pseudomonas aeruginosa):
| Agent | Dose | Mechanism | Coverage |
|---|---|---|---|
| Piperacillin-Tazobactam | 4.5 g IV q6h (or 18 g/24h continuous infusion) | Beta-lactam + beta-lactamase inhibitor | Broad Gram-negative (including Pseudomonas), Gram-positive, anaerobes |
| Cefepime | 2 g IV q8h | 4th-generation cephalosporin | Broad Gram-negative (including Pseudomonas), Gram-positive |
| Meropenem | 1 g IV q8h | Carbapenem | Broadest spectrum (reserve for ESBL or resistant organisms) |
Piperacillin-Tazobactam is the preferred first-line agent in most centers due to broad coverage and lower resistance rates. [23]
Indications to Add Vancomycin (Gram-Positive Coverage)
Add Vancomycin 15-20 mg/kg IV q8-12h (target trough 15-20 mg/L) if:
- Hemodynamic instability (septic shock)
- Clinically suspected catheter-related bloodstream infection (CRBSI)
- Skin or soft tissue infection (cellulitis, abscess)
- Mucositis (grade 3-4, risk of Viridans strep)
- Known MRSA colonization
- Previous MRSA infection
- Hospital with high MRSA prevalence (>10% of S. aureus isolates)
Duration of Vancomycin:
- Discontinue after 48-72 hours if blood cultures negative and clinical improvement
- Continue if Gram-positive organism isolated or CRBSI confirmed
Indications for Aminoglycoside Addition
Add Gentamicin 5-7 mg/kg IV once daily or Amikacin 15-20 mg/kg IV once daily if:
- Septic shock (synergistic killing with beta-lactams)
- Ecthyma gangrenosum or suspected Pseudomonas bacteremia
- Known resistant Gram-negative organism
Caution: Nephrotoxic and ototoxic; use for ≤5 days, monitor renal function and drug levels
Carbapenem Escalation
Switch to Meropenem 1 g IV q8h if:
- Known or suspected ESBL-producing organism (E. coli, Klebsiella)
- Clinical deterioration despite 48-72 hours of piperacillin-tazobactam
- Documented resistance to first-line agent
- Severe sepsis/septic shock in units with high ESBL prevalence
Step 3: Low-Risk Outpatient Oral Therapy (MASCC ≥21)
Eligibility Criteria:
- MASCC score ≥21
- Hemodynamically stable
- No organ dysfunction
- Able to tolerate oral intake
- Reliable social support and transport
- Close outpatient follow-up available (daily review)
- Expected brief neutropenia (less than 7 days)
Oral Regimen:
- Ciprofloxacin 500-750 mg PO BD PLUS
- Amoxicillin-clavulanate 625 mg PO TDS
Alternative (Penicillin allergy):
- Levofloxacin 750 mg PO once daily PLUS
- Clindamycin 600 mg PO TDS
Follow-Up:
- Daily clinical review (outpatient clinic or community visit)
- Admission triggers: Hemodynamic instability, new symptoms, persistent fever >48 hours, clinical deterioration
Outcome: Outpatient management safe in carefully selected low-risk patients, with cure rates 85-95% and hospitalization rates less than 10%. [24]
Step 4: Persistent Fever (Day 4-7)
Definition: Fever (≥38°C) persisting beyond 96-120 hours of appropriate broad-spectrum antibiotics
Clinical Reassessment:
- Repeat history and physical examination: Search for occult sources (perianal, sinuses, catheter site, skin)
- Repeat blood cultures: Check for breakthrough bacteremia
- Review microbiology: Adjust antibiotics based on culture sensitivities
Imaging:
- CT Chest: Evaluate for invasive pulmonary aspergillosis (halo sign, nodules)
- CT Abdomen/Pelvis: If abdominal symptoms (typhlitis, hepatosplenic candidiasis, abscess)
- CT Sinuses: If sinus symptoms (invasive fungal sinusitis)
Empirical Antifungal Therapy:
Initiate empirical antifungal coverage if:
- Fever persists despite 4-7 days of broad-spectrum antibiotics
- Prolonged neutropenia (≥7 days, expected to continue)
- Clinical deterioration
- Radiological findings suggestive of fungal infection
First-Line Empirical Antifungal Agents:
| Agent | Dose | Spectrum | Indication |
|---|---|---|---|
| Caspofungin | 70 mg IV load, then 50 mg IV daily | Candida (including fluconazole-resistant), Aspergillus | Empirical therapy, candidemia |
| Voriconazole | 6 mg/kg IV q12h x 2 doses, then 4 mg/kg IV q12h | Aspergillus, Candida, many molds | Suspected/proven invasive aspergillosis |
| Liposomal Amphotericin B | 3-5 mg/kg IV daily | Broadest antifungal spectrum | Refractory fever, renal failure (voriconazole contraindicated) |
Choice Considerations:
- Caspofungin: Better tolerated, less nephrotoxic, preferred if renal impairment
- Voriconazole: Preferred if invasive aspergillosis suspected (better CNS penetration)
- Liposomal Amphotericin B: Broadest coverage, reserve for refractory cases or mucormycosis concern
Fungal Biomarker Monitoring:
- Galactomannan (twice weekly in high-risk patients)
- (1→3)-β-D-Glucan (serial measurements if empirical antifungal initiated)
Step 5: Granulocyte Colony-Stimulating Factor (G-CSF)
Filgrastim (G-CSF) 300 mcg SC daily or Pegfilgrastim 6 mg SC once stimulates neutrophil production and may shorten duration of neutropenia.
ASCO/IDSA Indications for G-CSF in Neutropenic Sepsis:
- Septic shock or multi-organ dysfunction
- Pneumonia with hypoxia
- Invasive fungal infection
- Profound neutropenia (ANC less than 0.1 × 10^9/L) with expected prolonged recovery
- Age >65 years with serious comorbidities
NOT Routinely Recommended:
- Uncomplicated neutropenic fever without high-risk features
- As a substitute for antibiotics
Timing: Initiate within 24-72 hours of presentation if high-risk criteria met. Neutrophil recovery typically occurs 3-5 days after G-CSF initiation. [25]
Step 6: Duration of Antibiotics and De-Escalation
If Microbiologically Documented Infection
- Adjust antibiotics to narrowest effective spectrum based on culture sensitivities
- Total duration: 10-14 days (or longer for deep-seated infections like pneumonia, meningitis)
- Continue until: Clinical resolution AND neutrophil recovery (ANC >0.5 × 10^9/L)
If Clinically Documented Infection (No Organism Isolated)
- Continue broad-spectrum antibiotics until afebrile for 48-72 hours AND clinical improvement
- Total duration: 7-14 days depending on clinical severity
- Continue until: Neutrophil recovery (ANC >0.5 × 10^9/L)
If No Documented Infection (Fever of Unknown Origin)
Low-Risk Patients (MASCC ≥21):
- If afebrile for 48 hours, clinically well, and cultures negative: Discontinue antibiotics
- Close outpatient follow-up
High-Risk Patients (MASCC less than 21):
- If afebrile for 48-72 hours and clinically stable: Consider discontinuing antibiotics if ANC recovering
- If persistent neutropenia (ANC less than 0.5), many clinicians continue prophylactic antibiotics (fluoroquinolone)
Step 7: Catheter Management
Indications for Central Line Removal:
- Tunnel infection (erythema, induration along catheter tract)
- Port pocket infection
- Bacteremia with Staphylococcus aureus, Pseudomonas aeruginosa, Candida species, or other difficult-to-treat organisms
- Persistent bacteremia despite 72 hours of appropriate antibiotics
Catheter Salvage (with antibiotic lock therapy):
- Coagulase-negative staphylococci (if clinically stable)
- Single lumen involved, catheter essential for treatment
7. Prognosis and Complications
Mortality Determinants
| Factor | Low Mortality | High Mortality |
|---|---|---|
| MASCC Score | ≥21 (1-3%) | less than 21 (10-40%) |
| Hemodynamics | Normotensive (2-5%) | Septic shock (40-60%) |
| Underlying Malignancy | Solid tumor (1-5%) | Hematologic malignancy (10-15%) |
| Neutropenia Depth | ANC 0.2-0.5 (5-10%) | ANC less than 0.1 (20-30%) |
| Neutropenia Duration | less than 7 days (5%) | ≥10 days (15-25%) |
| Door-to-Antibiotic Time | less than 60 minutes (5-10%) | >6 hours (30-50%) |
| Organism | Gram-positive (5-10%) | Gram-negative with MDR (20-40%) |
| Complication | None (2-5%) | Invasive fungal infection (30-50%) |
Major Complications
1. Septic Shock (5-10% of FN cases)
- Persistent hypotension despite fluid resuscitation
- Multi-organ dysfunction (AKI, ARDS, DIC)
- Mortality: 40-60%
- Management: ICU, vasopressors, mechanical ventilation, RRT
2. Invasive Fungal Infection (IFI)
Risk Factors:
- Prolonged neutropenia (>10 days)
- High-dose corticosteroids
- Graft-versus-host disease (GVHD)
- Previous IFI
- Broad-spectrum antibiotics
Invasive Pulmonary Aspergillosis:
- Nodules, halo sign on CT
- Mortality: 30-50% (higher if delayed diagnosis)
- Treatment: Voriconazole or liposomal amphotericin B
Candidemia:
- Central line-associated
- Mortality: 20-40%
- Treatment: Echinocandin (caspofungin), remove central line, ophthalmology review (endophthalmitis)
3. Typhlitis (Neutropenic Enterocolitis)
- RLQ pain, fever, bloody diarrhea
- Bowel wall thickening on CT
- Complications: Perforation, peritonitis, shock
- Mortality: 30-50%
- Management: Bowel rest, NG decompression, broad-spectrum antibiotics (including anaerobic coverage), surgical consultation
4. Clostridium difficile Colitis
- Diarrhea, abdominal pain, leukocytosis (if neutrophils recovering)
- C. difficile toxin positive
- Management: Vancomycin 125 mg PO QDS or Fidaxomicin 200 mg PO BD
5. Acute Respiratory Distress Syndrome (ARDS)
- Associated with Viridans streptococcal bacteremia and severe mucositis
- Bilateral infiltrates, PaO2/FiO2 less than 300
- Mortality: 40-60%
- Management: Lung-protective ventilation, prone positioning, ECMO if refractory
Long-Term Sequelae
- Recurrent neutropenic episodes: 20-30% of patients experience multiple FN episodes during chemotherapy course
- Chemotherapy dose delays: FN may necessitate dose reduction or schedule delays, potentially compromising cancer cure rates
- Psychological impact: Anxiety, fear of infection, reduced quality of life
8. Prevention
Primary Prophylaxis (Before First Chemotherapy Cycle)
1. G-CSF Prophylaxis
ASCO/EORTC Guidelines: Administer G-CSF if chemotherapy regimen has >20% risk of febrile neutropenia.
Agents:
- Filgrastim 300 mcg SC daily (starting 24-72 hours post-chemotherapy, continue until ANC >10 × 10^9/L or for 10-14 days)
- Pegfilgrastim 6 mg SC once (24-72 hours post-chemotherapy)
Benefit: Reduces FN incidence by 50%, allows chemotherapy dose intensity maintenance, reduces FN-related mortality.
2. Antibiotic Prophylaxis
Fluoroquinolone Prophylaxis (Ciprofloxacin 500 mg PO BD or Levofloxacin 500 mg PO once daily):
Indications:
- Expected profound neutropenia (ANC less than 0.1 × 10^9/L) for ≥7 days
- Hematologic malignancy undergoing intensive chemotherapy or HSCT
Benefits: Reduces risk of Gram-negative bacteremia and all-cause mortality by 30-50%.
Risks: Promotes fluoroquinolone resistance, Clostridium difficile infection, disrupts microbiome. [26]
Controversy: Not universally recommended due to resistance concerns.
3. Antifungal Prophylaxis
Posaconazole 300 mg PO once daily or Fluconazole 400 mg PO once daily:
Indications:
- High-risk hematologic malignancy: Acute leukemia, allogeneic HSCT, graft-versus-host disease
- Expected prolonged neutropenia (>10 days)
Benefits: Reduces invasive fungal infection incidence and IFI-related mortality. [27]
4. Viral Prophylaxis
Aciclovir 400 mg PO BD or Valaciclovir 500 mg PO BD:
Indications:
- Seropositive for HSV or VZV
- Allogeneic HSCT recipients
Secondary Prophylaxis (After FN Episode)
- G-CSF in subsequent chemotherapy cycles (if FN occurred in prior cycle)
- Dose reduction of chemotherapy (if FN recurrent despite G-CSF)
- Antibiotic prophylaxis (if recurrent episodes)
Patient Education
Neutropenic Precautions:
- Avoid crowds and close contact with sick individuals
- Hand hygiene (soap and water or alcohol gel)
- Oral hygiene (soft toothbrush, saline mouthwash)
- Avoid raw or undercooked foods (Listeria, Salmonella risk)
- Avoid gardening and soil exposure (Aspergillus spores)
- Promptly report fever (>38°C) to oncology team
9. Single Best Answer (SBA) Questions
Question 1
A 52-year-old woman with newly diagnosed AML is Day 10 post-induction chemotherapy (cytarabine + daunorubicin). She presents to the Emergency Department with fever (38.7°C). Blood tests reveal: WBC 0.8 × 10^9/L, neutrophils 0.1 × 10^9/L, platelets 20 × 10^9/L. She is hemodynamically stable (BP 120/70 mmHg, HR 90 bpm). What is the single most appropriate immediate management?
- A) Oral ciprofloxacin and amoxicillin-clavulanate, discharge with daily outpatient review
- B) IV piperacillin-tazobactam within 60 minutes, admit for monitoring
- C) IV piperacillin-tazobactam + vancomycin + gentamicin
- D) Await blood culture results before starting antibiotics
- E) Subcutaneous G-CSF, then IV antibiotics once neutrophils recover
Answer: B
Explanation: This patient has high-risk febrile neutropenia (hematologic malignancy, profound neutropenia ANC 0.1, inpatient onset). MASCC score is less than 21 (hematologic malignancy = 0 points). She requires immediate empirical IV broad-spectrum antibiotics (piperacillin-tazobactam is first-line antipseudomonal coverage) within 60 minutes and inpatient admission. Option A (oral outpatient therapy) is inappropriate for high-risk patients. Option C (triple therapy) is excessive for initial management in a hemodynamically stable patient without specific indications for vancomycin or aminoglycoside. Option D (awaiting cultures) is dangerous; every hour of delay increases mortality. Option E misunderstands that G-CSF is adjunctive, not a substitute for antibiotics, and neutrophil recovery takes 3-5 days.
Question 2
A 67-year-old man with metastatic colon cancer is receiving FOLFOX chemotherapy. He develops fever (38.5°C) 9 days post-cycle. ANC is 0.4 × 10^9/L. He is started on IV piperacillin-tazobactam. After 5 days, he remains febrile (38.2°C) despite broad-spectrum antibiotics. Blood cultures are negative. He has developed a dry cough and mild dyspnea (SpO2 93% on room air). What is the most appropriate next investigation?
- A) Chest X-ray
- B) High-resolution CT chest
- C) Bronchoscopy with bronchoalveolar lavage
- D) Serum procalcitonin
- E) Repeat blood cultures
Answer: B
Explanation: This patient has persistent fever (day 5) despite broad-spectrum antibiotics, with new respiratory symptoms. In neutropenic patients with suspected pneumonia, chest X-ray has low sensitivity because the absence of neutrophils prevents lobar consolidation. High-resolution CT chest is the investigation of choice; it can detect subtle findings like ground-glass opacities, nodules, or the pathognomonic "halo sign" of early invasive pulmonary aspergillosis. Option A (CXR) may be falsely negative. Option C (bronchoscopy) is premature; imaging should guide the need for invasive sampling. Options D and E do not address the likely pulmonary fungal infection.
Question 3
What is the molecular mechanism underlying the absence of lobar consolidation on chest X-ray in a severely neutropenic patient with bacterial pneumonia?
- A) The bacteria do not proliferate in alveolar spaces
- B) Impaired CXCL8 (IL-8)-mediated neutrophil recruitment prevents pus formation
- C) Lack of TNF-α and IL-1β cytokine production
- D) Alveolar macrophages are sufficient to control infection
- E) The infection is confined to the interstitium
Answer: B
Explanation: Lobar consolidation on chest X-ray is primarily the radiographic appearance of neutrophil-rich inflammatory exudate (pus) and fibrin filling the alveolar spaces. In severe neutropenia, tissue macrophages detect bacterial PAMPs and release chemokines (CXCL8/IL-8), but there are no circulating neutrophils to recruit. Without neutrophil influx, there is no pus formation, and the chest X-ray appears clear despite potentially lethal parenchymal infection. Option C is incorrect; cytokines (TNF-α, IL-1β) are still produced by macrophages and are responsible for the fever. Option D is incorrect; alveolar macrophages alone are insufficient to control bacterial proliferation.
Question 4
A 45-year-old woman with lymphoma is admitted with neutropenic sepsis (ANC 0.2 × 10^9/L, temperature 39°C). She is started on IV piperacillin-tazobactam. Blood cultures subsequently grow Staphylococcus epidermidis from both the central line and peripheral cultures. She is hemodynamically stable and afebrile after 48 hours of antibiotics. What is the most appropriate antibiotic modification?
- A) Continue piperacillin-tazobactam alone (adequate Gram-positive coverage)
- B) Add vancomycin, continue piperacillin-tazobactam
- C) Switch to vancomycin monotherapy
- D) Add linezolid instead of vancomycin
- E) Discontinue all antibiotics (likely contaminant)
Answer: B
Explanation: Staphylococcus epidermidis (coagulase-negative staphylococcus) isolated from both central line and peripheral blood cultures indicates catheter-related bloodstream infection (CRBSI), not contamination. Piperacillin-tazobactam has Gram-positive activity but vancomycin is preferred for CoNS due to frequent methicillin resistance and biofilm-associated infections. Add vancomycin (targeting CoNS) and continue piperacillin-tazobactam (covering Gram-negative organisms, as this is neutropenic sepsis with no organism confirmation for Gram-negative exclusion). Option C (vancomycin monotherapy) is inappropriate; must maintain Gram-negative coverage in neutropenic sepsis. Option E is dangerous; positive cultures from two sites (especially central + peripheral) confirm true bacteremia, not contamination.
Question 5
A 58-year-old man with AML is Day 12 post-chemotherapy with profound neutropenia (ANC 0.05 × 10^9/L). He develops severe right lower quadrant abdominal pain, distension, and bloody diarrhea. Temperature is 38.9°C, BP 95/60 mmHg, HR 115 bpm. On examination, there is marked RLQ tenderness and guarding. What is the single most likely diagnosis and most appropriate immediate management?
- A) Acute appendicitis; surgical appendectomy
- B) Clostridium difficile colitis; start oral vancomycin
- C) Typhlitis (neutropenic enterocolitis); bowel rest, IV broad-spectrum antibiotics including anaerobic coverage, surgical consultation
- D) Ischemic colitis; IV fluids and anticoagulation
- E) Graft-versus-host disease of the gut; start high-dose corticosteroids
Answer: C
Explanation: Typhlitis (neutropenic enterocolitis) is inflammation and necrosis of the cecum and ascending colon occurring in profoundly neutropenic patients. The classic triad is fever, RLQ pain, and neutropenia. Bloody diarrhea and shock are common. CT abdomen shows bowel wall thickening (>4 mm), pericolic stranding. Management is medical: bowel rest (NPO), NG decompression, IV broad-spectrum antibiotics including anaerobic coverage (e.g., piperacillin-tazobactam or meropenem + metronidazole), and surgical consultation (for potential perforation or peritonitis). Surgery is generally avoided unless perforation or peritonitis occurs. Option A (appendectomy) is inappropriate; surgery in severe neutropenia has high morbidity/mortality. Option E is incorrect; this patient has not undergone allogeneic HSCT (AML induction chemotherapy), so GVHD is not applicable.
10. Viva Voce Scenarios
Scenario 1: The Persistent Fever
Examiner: "A 60-year-old woman with AML is Day 8 post-induction chemotherapy. Her ANC is 0.08 × 10^9/L. She has been on IV piperacillin-tazobactam for 96 hours for febrile neutropenia but continues to spike fevers (39°C). Blood cultures remain negative. She has no respiratory, abdominal, or urinary symptoms. What is your management approach?"
Candidate Response:
-
Reassessment:
- I would perform a thorough repeat clinical examination, specifically searching for occult sources: oral cavity (mucositis), skin (catheter site, perianal region), sinuses, and subtle respiratory signs.
- Review recent blood tests: inflammatory markers (CRP), renal/hepatic function, and ensure no breakthrough neutrophil recovery (which might unmask an abscess).
-
Imaging:
- Order high-resolution CT chest to look for invasive pulmonary aspergillosis (halo sign, nodules, air-crescent sign) even in the absence of respiratory symptoms, as fungal pneumonia may be clinically silent.
- If abdominal symptoms develop, CT abdomen/pelvis to exclude typhlitis, hepatosplenic candidiasis, or abscess.
-
Microbiological Escalation:
- Send fungal biomarkers: serum galactomannan and (1→3)-β-D-glucan.
- Repeat blood cultures (aerobic, anaerobic, fungal).
-
Empirical Antifungal Therapy:
- Given persistent fever for 96 hours and prolonged neutropenia (ANC 0.08, expected to continue), I would initiate empirical antifungal therapy.
- I would start an echinocandin (e.g., caspofungin 70 mg IV load, then 50 mg daily) or voriconazole (6 mg/kg IV q12h x 2, then 4 mg/kg q12h), depending on institutional protocols and suspicion of aspergillosis.
-
Consider Antibiotic Escalation:
- If there is clinical deterioration or concern for resistant Gram-negative organisms (ESBL), I would escalate to a carbapenem (meropenem 1 g IV q8h).
-
G-CSF:
- Given profound neutropenia and persistent fever, I would consider adding G-CSF (filgrastim 300 mcg SC daily) to accelerate neutrophil recovery.
Examiner: "Good. The galactomannan comes back at ODI 0.8 (positive), and CT chest shows a nodule with a halo sign. What now?"
Candidate: "This confirms invasive pulmonary aspergillosis. I would switch to voriconazole (if not already started) as it has superior efficacy for aspergillosis compared to echinocandins. I would also arrange bronchoscopy with BAL for fungal culture and PCR if the patient is stable enough to tolerate the procedure, as microbiological confirmation guides duration of therapy. Treatment duration is typically at least 12 weeks, and I would monitor serial galactomannan levels and repeat imaging to assess response."
Scenario 2: The Hypotensive Patient
Examiner: "A 72-year-old man with metastatic lung cancer is Day 10 post-chemotherapy. He presents with fever (38.6°C), ANC 0.3 × 10^9/L, BP 85/50 mmHg, HR 120 bpm, lactate 4.2 mmol/L. How do you manage him?"
Candidate Response:
-
Recognize Septic Shock:
- This patient has neutropenic septic shock (fever + neutropenia + hypotension + lactate >4). This is a medical emergency with mortality >40%.
-
Immediate Resuscitation (Sepsis Six within 1 hour):
- Oxygen: High-flow oxygen to maintain SpO2 >94%
- IV Fluid Resuscitation: 30 mL/kg crystalloid bolus (e.g., 2 liters Hartmann's) within the first hour
- Blood Cultures: Two sets (peripheral + central line if present) before antibiotics, but do not delay antibiotics
- Empirical Antibiotics: Immediate broad-spectrum IV antibiotics:
- Piperacillin-tazobactam 4.5 g IV (antipseudomonal beta-lactam)
- Add vancomycin 15-20 mg/kg IV (Gram-positive coverage given shock)
- Add gentamicin 5-7 mg/kg IV (synergistic killing in septic shock)
- Measure Lactate: Already done (4.2 mmol/L)
- Monitor Urine Output: Insert urinary catheter, target >0.5 mL/kg/hr
-
Escalate to ICU:
- This patient requires ICU admission for close hemodynamic monitoring and likely vasopressor support.
- If hypotension persists despite 30 mL/kg fluid resuscitation, start norepinephrine infusion via central line (target MAP ≥65 mmHg).
-
Additional Investigations:
- Full septic screen: blood cultures, urine culture, CXR (or HRCT chest if respiratory symptoms)
- Renal function, liver function, coagulation (DIC screen)
- Echocardiography if concerns about cardiac function
-
G-CSF:
- Given septic shock, I would administer filgrastim 300 mcg SC to accelerate neutrophil recovery.
-
Source Control:
- Examine for removable sources (indwelling catheters, abscess). If central line infection suspected and patient unstable, consider line removal after blood cultures obtained.
Examiner: "He stabilizes after fluids and norepinephrine. Blood cultures at 48 hours grow Pseudomonas aeruginosa sensitive to piperacillin-tazobactam but resistant to ciprofloxacin. What changes do you make?"
Candidate: "I would continue piperacillin-tazobactam as it has documented sensitivity and is appropriate for Pseudomonas. I would discontinue vancomycin (no Gram-positive organism isolated) and discontinue gentamicin after 3-5 days to minimize nephrotoxicity and ototoxicity. I would continue antibiotics for a total of 14 days (or until neutrophil recovery and clinical resolution), as Pseudomonas bacteremia has high relapse risk if treated briefly."
Scenario 3: The Outpatient Dilemma
Examiner: "A 50-year-old woman with breast cancer is receiving adjuvant chemotherapy (docetaxel + cyclophosphamide). She is Day 9 post-cycle and presents to the Emergency Department with fever (38.4°C). Her ANC is 0.6 × 10^9/L. She is otherwise well: no symptoms, BP 125/75 mmHg, HR 85 bpm, SpO2 98% on air. You calculate her MASCC score as 23. Can you send her home with oral antibiotics?"
Candidate Response:
MASCC Score Assessment:
- Her MASCC score is 23, which categorizes her as low-risk (threshold ≥21). This suggests outpatient oral therapy might be appropriate.
However, I would assess additional eligibility criteria for outpatient management:
- Clinical Stability: She is hemodynamically stable, no organ dysfunction, no respiratory or other symptoms. ✓
- Solid Tumor: She has breast cancer (solid tumor), which is lower risk than hematologic malignancy. ✓
- Ability to Tolerate Oral Intake: She can swallow medications. ✓
- Expected Duration of Neutropenia: Docetaxel + cyclophosphamide typically causes nadir at 7-10 days with recovery by day 14-21. Expected brief neutropenia (less than 7 days). ✓
- Social Support and Access: I would confirm she has reliable transport, phone access, and someone at home, and can return daily for review. Must confirm.
- Patient Understanding and Compliance: She understands the need to return immediately if symptoms worsen (hypotension, dyspnea, confusion, persistent fever). Must confirm.
If all criteria met:
- I would prescribe oral ciprofloxacin 500-750 mg BD plus amoxicillin-clavulanate 625 mg TDS.
- Arrange daily outpatient review (clinic or community visit) for clinical assessment and blood tests.
- Provide clear safety-netting: Return immediately if BP drops, shortness of breath, confusion, vomiting, or fever persists >48 hours.
If any doubt (e.g., poor social support, unreliable follow-up, patient anxiety):
- I would admit for IV piperacillin-tazobactam and observation for 24-48 hours, then reassess for early discharge.
Examiner: "She returns the next day. She remains febrile (38.1°C) and has developed a cough. What now?"
Candidate: "This represents clinical deterioration (new respiratory symptoms). Outpatient management is no longer appropriate. I would admit her for inpatient IV antibiotics (piperacillin-tazobactam), perform a high-resolution CT chest to exclude neutropenic pneumonia or invasive fungal infection, and closely monitor her clinical status."
11. Patient Explanation (Layperson Summary)
"Because of your chemotherapy, the white blood cells in your blood—your body's internal soldiers that fight off infections—are currently at a very low level. This means your body can't defend itself against germs that normally live on your skin or in your gut without causing any harm.
A fever is the first and sometimes the only warning sign that an infection is starting. That's why we treat a fever in your situation as a medical emergency. We give you strong antibiotics through a drip immediately—we don't wait for test results to come back, because in this situation, every hour counts. Delaying treatment even by a few hours can significantly increase the risk.
Over the next few days, we'll monitor you closely and adjust the treatment based on how you respond and what the tests show. Most people recover well with prompt treatment, and your white blood cell count will gradually rise as your bone marrow recovers from the chemotherapy.
If you develop a fever at home (temperature over 38°C), you must contact your oncology team or come to the hospital immediately—do not wait."
12. Summary: Key Exam Takeaways
Must-Know Facts for MRCP
-
Definition: Fever (≥38.3°C single or ≥38°C sustained) + ANC less than 0.5 × 10^9/L.
-
Time-Critical Emergency: Antibiotics within 60 minutes; every hour of delay increases mortality by 18-20%.
-
First-Line Antibiotics: Piperacillin-tazobactam 4.5 g IV (antipseudomonal coverage is essential).
-
Add Vancomycin If: Shock, catheter infection, skin/soft tissue infection, MRSA colonization, or severe mucositis.
-
MASCC Score: ≥21 = low-risk (eligible for outpatient oral therapy); less than 21 = high-risk (inpatient IV therapy).
-
Persistent Fever (Day 4-7): Initiate empirical antifungal therapy (caspofungin or voriconazole).
-
"Cryptic Infection": Absence of pus, consolidation, or localizing signs due to lack of neutrophils.
-
Red Flags:
- Ecthyma gangrenosum = Pseudomonas bacteremia
- RLQ pain = Typhlitis (neutropenic enterocolitis)
- Halo sign on CT = Invasive aspergillosis
-
G-CSF Indications: Septic shock, pneumonia, invasive fungal infection, profound neutropenia, age >65.
-
Prevention: G-CSF prophylaxis if chemotherapy regimen has >20% FN risk; fluoroquinolone prophylaxis in high-risk hematologic patients.
13. References
-
Taplitz RA, Kennedy EB, Bow EJ, et al. Antimicrobial Prophylaxis for Adult Patients With Cancer-Related Immunosuppression: ASCO and IDSA Clinical Practice Guideline Update. J Clin Oncol. 2018;36(30):3043-3054. [PMID: 30074509]
-
Kuderer NM, Dale DC, Crawford J, et al. Mortality, morbidity, and cost associated with febrile neutropenia in adult cancer patients. Cancer. 2006;106(10):2258-2266. [PMID: 16575919]
-
Rosa RG, Goldani LZ. Cohort study of the impact of time to antibiotic administration on mortality in patients with febrile neutropenia. Antimicrob Agents Chemother. 2014;58(7):3799-3803. [PMID: 24752266]
-
Klastersky J, Ameye L, Maertens J, et al. Bacteraemia in febrile neutropenic cancer patients. Int J Antimicrob Agents. 2007;30(Suppl 1):S51-S59. [PMID: 17689935]
-
Bow EJ. Infection in neutropenic patients with cancer. Crit Care Clin. 2013;29(3):411-441. [PMID: 23830647]
-
Freifeld AG, Bow EJ, Sepkowitz KA, et al. Clinical Practice Guideline for the Use of Antimicrobial Agents in Neutropenic Patients with Cancer: 2010 Update by the Infectious Diseases Society of America. Clin Infect Dis. 2011;52(4):e56-e93. [PMID: 21258094]
-
National Comprehensive Cancer Network (NCCN). Prevention and Treatment of Cancer-Related Infections. Version 1.2024. Available at: https://www.nccn.org/guidelines
-
Weycker D, Li X, Edelsberg J, et al. Risk and consequences of chemotherapy-induced febrile neutropenia in patients with metastatic solid tumors. J Oncol Pract. 2015;11(1):47-54. [PMID: 25466711]
-
Pagano L, Caira M, Nosari A, et al. Fungal infections in recipients of hematopoietic stem cell transplants: results of the SEIFEM B-2004 study. Clin Infect Dis. 2007;45(9):1161-1170. [PMID: 17918077]
-
Kontoyiannis DP, Marr KA, Park BJ, et al. Prospective surveillance for invasive fungal infections in hematopoietic stem cell transplant recipients, 2001-2006: overview of the Transplant-Associated Infection Surveillance Network (TRANSNET) Database. Clin Infect Dis. 2010;50(8):1091-1100. [PMID: 20218877]
-
Bodey GP, Buckley M, Sathe YS, Freireich EJ. Quantitative relationships between circulating leukocytes and infection in patients with acute leukemia. Ann Intern Med. 1966;64(2):328-340. [PMID: 5216294]
-
Elting LS, Cooksley CD, Chambers MS, Garden AS. Risk, outcomes, and costs of radiation-induced oral mucositis among patients with head-and-neck malignancies. Int J Radiat Oncol Biol Phys. 2007;68(4):1110-1120. [PMID: 17398022]
-
Viscoli C, Varnier O, Machetti M. Infections in patients with febrile neutropenia: epidemiology, microbiology, and risk stratification. Clin Infect Dis. 2005;40(Suppl 4):S240-S245. [PMID: 15768331]
-
Hotchkiss RS, Monneret G, Payen D. Sepsis-induced immunosuppression: from cellular dysfunctions to immunotherapy. Nat Rev Immunol. 2013;13(12):862-874. [PMID: 24232462]
-
Singer M, Deutschman CS, Seymour CW, et al. The Third International Consensus Definitions for Sepsis and Septic Shock (Sepsis-3). JAMA. 2016;315(8):801-810. [PMID: 26903338]
-
Keng MK, Sekeres MA. Febrile neutropenia in hematologic malignancies. Curr Hematol Malig Rep. 2013;8(4):370-378. [PMID: 24146092]
-
Heussel CP, Kauczor HU, Heussel GE, et al. Pneumonia in febrile neutropenic patients and in bone marrow and blood stem-cell transplant recipients: use of high-resolution computed tomography. J Clin Oncol. 1999;17(3):796-805. [PMID: 10071270]
-
Gorschlüter M, Mey U, Strehl J, et al. Neutropenic enterocolitis in adults: systematic analysis of evidence quality. Eur J Haematol. 2005;75(1):1-13. [PMID: 15946304]
-
Klastersky J, Paesmans M, Rubenstein EB, et al. The Multinational Association for Supportive Care in Cancer risk index: A multinational scoring system for identifying low-risk febrile neutropenic cancer patients. J Clin Oncol. 2000;18(16):3038-3051. [PMID: 10944139]
-
Shapiro NI, Howell MD, Talmor D, et al. Serum lactate as a predictor of mortality in emergency department patients with infection. Ann Emerg Med. 2005;45(5):524-528. [PMID: 15855951]
-
Robinson JO, Lamoth F, Bally F, et al. Monitoring procalcitonin in febrile neutropenia: what is its utility for initial diagnosis of infection and reassessment of antimicrobial therapy? PLoS One. 2011;6(4):e18886. [PMID: 21533119]
-
Carmona-Bayonas A, Gómez J, González-Billalabeitia E, et al. Prognostic evaluation of febrile neutropenia in apparently stable adult cancer patients. Br J Cancer. 2011;105(5):612-617. [PMID: 21829202]
-
Paul M, Dickstein Y, Schlesinger A, et al. Beta-lactam versus beta-lactam-aminoglycoside combination therapy in cancer patients with neutropenia. Cochrane Database Syst Rev. 2013;(6):CD003038. [PMID: 23760787]
-
Vidal L, Ben-Dor I, Paul M, et al. Oral versus intravenous antibiotic treatment for febrile neutropenia in cancer patients. Cochrane Database Syst Rev. 2013;(10):CD003992. [PMID: 24105485]
-
Smith TJ, Bohlke K, Lyman GH, et al. Recommendations for the Use of WBC Growth Factors: American Society of Clinical Oncology Clinical Practice Guideline Update. J Clin Oncol. 2015;33(28):3199-3212. [PMID: 26169616]
-
Bucaneve G, Micozzi A, Menichetti F, et al. Levofloxacin to prevent bacterial infection in patients with cancer and neutropenia. N Engl J Med. 2005;353(10):977-987. [PMID: 16148283]
-
Cornely OA, Maertens J, Winston DJ, et al. Posaconazole vs. fluconazole or itraconazole prophylaxis in patients with neutropenia. N Engl J Med. 2007;356(4):348-359. [PMID: 17251531]
Last Updated: 2026-01-06 | MedVellum Editorial Team Citation Count: 24 Target Examination: MRCP, FRACP, MRCS (Emergency Oncology/Haematology)
Frequently asked questions
Quick clarifications for common clinical and exam-facing questions.
When should I seek emergency care for neutropenic sepsis?
Seek immediate emergency care if you experience any of the following warning signs: Systolic BP less than 90 mmHg (Septic Shock), Ecthyma gangrenosum (Black necrotic skin lesions - Pseudomonas), RLQ pain and distension (Typhlitis/Neutropenic Enterocolitis), New-onset hypoxia or 'Halo sign' on CT (Invasive Aspergillosis), Altered mental status or meningism, Perianal pain/abscess in neutropenic patient, ANC less than 0.1 x 10^9/L with expected prolonged neutropenia.
Learning map
Use these linked topics to study the concept in sequence and compare related presentations.
Prerequisites
Start here if you need the foundation before this topic.
- Chemotherapy Principles
- Sepsis Pathophysiology
Differentials
Competing diagnoses and look-alikes to compare.
- Tumour Lysis Syndrome
- Graft Versus Host Disease
- Drug Fever
Consequences
Complications and downstream problems to keep in mind.
- Typhlitis
- Invasive Fungal Infection
- Septic Shock