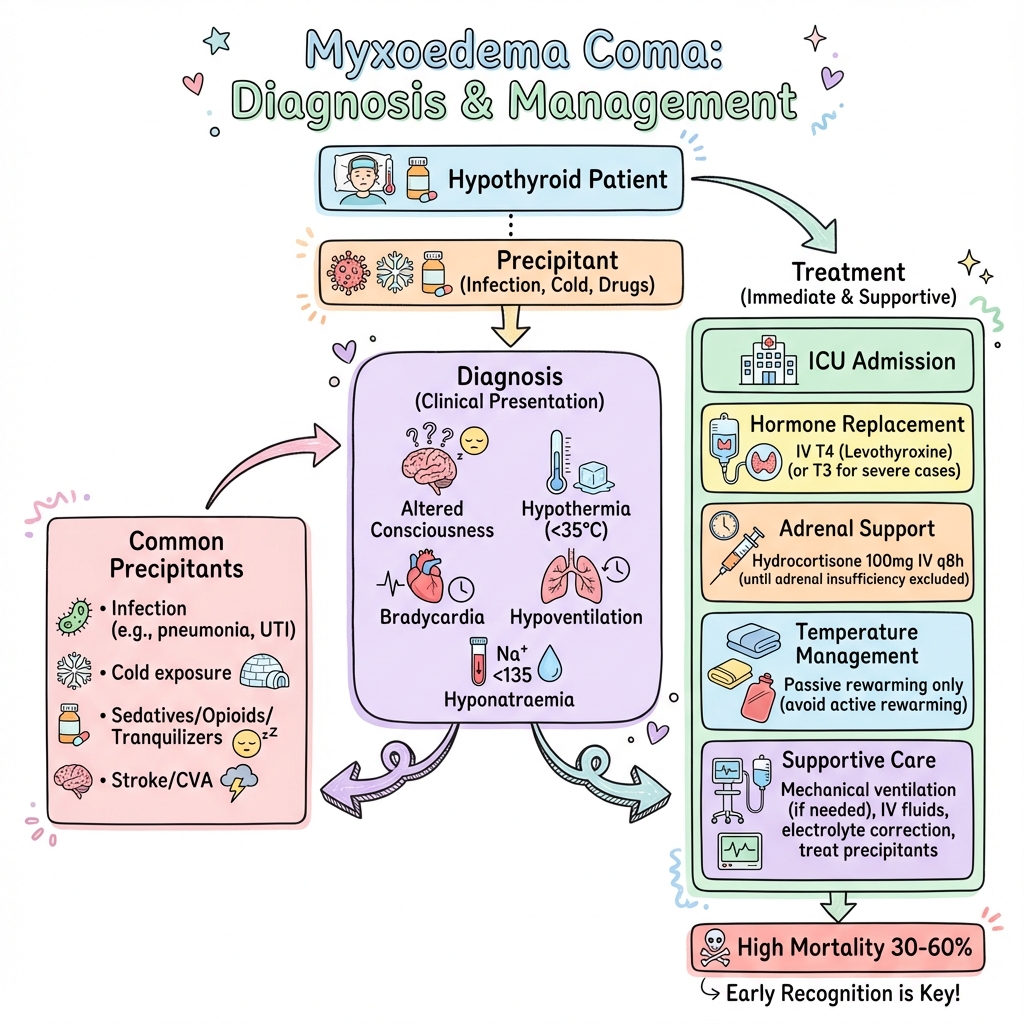
Myxoedema Coma
Key Facts The "Winter Peak" : Over 90% of cases occur during winter months due to cold-induced stress on minimal thermogenic reserves. The T4-T3 Block : In severe illness, the peripheral conversion of T4 to active T3...
What matters first
Key Facts The "Winter Peak" : Over 90% of cases occur during winter months due to cold-induced stress on minimal thermogenic reserves. The T4-T3 Block : In severe illness, the peripheral conversion of T4 to active T3...
Altered mental status (obtundation to coma)
4 Jan 2026
Generated educational material; verify before clinical use.
Visible references section
See the concept before reading it
Study the key anatomy, imaging, and decision pathways as full teaching plates.
Clinical board
A visual summary of the highest-yield teaching signals on this page.
Urgent signals
Safety-critical features pulled from the topic metadata.
- Altered mental status (obtundation to coma)
- Core temperature less than 35.0CC (Hypothermia)
- Severe bradycardia and hypotension (Shock)
- Hypoventilation (Hypercapnic respiratory failure)
Linked comparisons
Differentials and adjacent topics worth opening next.
- Adrenal Crisis
- Severe Hyponatraemia
Content status and exam context
This page is AI-generated educational content. It may contain errors or omissions and is not a substitute for current guidelines, local protocols, senior clinical judgement, or professional medical advice.
MedVellum does not claim an individual clinician reviewer, board certification, or professional credential for this page unless a future version names a real, verifiable reviewer.
Topic family
This concept exists in multiple MedVellum libraries. Use the primary page for the broadest reference view and the others for exam-specific framing.
Key Facts The "Winter Peak" : Over 90% of cases occur during winter months due to cold-induced stress on minimal thermogenic reserves. The T4-T3 Block : In severe illness, the peripheral conversion of T4 to active T3...
Myxoedema coma represents the most severe manifestation of decompensated hypothyroidism with mortality rates of 25-60% e... ACEM Fellowship Written, ACEM Fellow
Myxoedema coma (myxedema crisis) is the extreme decompensated state of hypothyroidism with mortality 20-60% despite inte... ACEM Primary Written, ACEM Primary V
Clinical explanation and evidence
Myxoedema Coma: V4 Gold Standard Guide
1. Summary
Myxoedema Coma (MC) is the most severe, life-threatening manifestation of decompensated hypothyroidism, representing a global collapse of homeostatic mechanisms. [1] Despite the name, most patients present with obtundation or lethargy rather than frank coma. [2] The condition is a "physiological hibernation" state characterized by the cardinal triad of altered mental status, hypothermia, and a precipitating event (most commonly infection or cold exposure). [3] The pathophysiology involves a catastrophic downregulation of mitochondrial activity and the Na+/K+ ATPase pump, leading to multisystem failure including hypercapnic respiratory failure, bradycardic shock, and dilutional hyponatraemia. [4,10] Mortality remains high (30-60%) and is heavily dependent on early clinical recognition before laboratory confirmation. [5] Management is strictly protocol-driven, requiring high-dose IV Levothyroxine (T4), IV Liothyronine (T3), and mandatory empirical Hydrocortisone to prevent adrenal crisis. [1,6]
2. Key Facts
- The "Winter Peak": Over 90% of cases occur during winter months due to cold-induced stress on minimal thermogenic reserves. [2,11]
- The T4-T3 Block: In severe illness, the peripheral conversion of T4 to active T3 is inhibited (Type 1 deiodinase failure), necessitating the use of IV T3 in deep coma. [4,15]
- The "Steroid First" Mandate: Thyroid hormone replacement must be preceded or accompanied by Hydrocortisone to prevent precipitating a fatal adrenal crisis. [1,12]
- Non-Osmotic Vasopressin: Hyponatraemia is driven by low cardiac output and decreased GFR, triggering non-osmotic ADH release (SIADH-like state). [7,17]
- Passive Rewarming Only: Active rewarming is contraindicated as it causes rapid peripheral vasodilation and cardiovascular collapse ("rewarming shock"). [1,8]
- The 80% Female Rule: MC reflects the underlying epidemiology of Hashimoto's thyroiditis, predominantly affecting elderly women. [11]
3. Clinical Pearls
The "Rectal Probe" Rule: Standard electronic thermometers often cannot measure below 34°C. In a suspected MC case, a low-reading rectal probe is mandatory to detect profound hypothermia (less than 30°C), which is a key prognostic marker. [1,5]
The "GCS Trap": Do not wait for a GCS of 3. Any patient with hypothyroidism and any change in affect, confusion, or slowed speech in the presence of an infection should be treated as "impending" myxoedema coma. [3]
The "Macroglossia" Airway: Myxoedema (glycosaminoglycan deposition) in the tongue and vocal cords makes intubation technically difficult and increases the risk of upper airway obstruction. [4]
The "Slow-Release" Reflex: Delayed relaxation of the Achilles tendon reflex (Hertoghe's sign) is highly specific for severe hypothyroidism and can be elicited even in the semi-comatose patient. [11]
4. Epidemiology
- Incidence: Extremely rare, affecting ~0.22 per million people per year. [11]
- Mortality: 30-50% in modern series; mortality is driven by age > 70, core temp less than 30°C, and persistent bradycardia. [5,13]
- The "Typical" Patient: 80% are women, mean age 70, presenting in December-February. [2]
- Central Hypothyroidism: Only 5% of cases are secondary (pituitary); these patients lack a goitre and have other pituitary deficiencies (ACTH/LH/FSH). [1]
5. 7-Step Molecular Pathophysiology
Step 1: Loss of Genomic T3 Signaling
Thyroid hormone (T3) normally binds to nuclear receptors (TRα, TRβ), promoting the transcription of the Na+/K+ ATPase pump and mitochondrial uncoupling proteins (UCPs). In MC, this genomic signaling stops, leading to immediate cellular energy failure. [4,30]
Step 2: The Na+/K+ ATPase Collapse
As the density of Na+/K+ pumps on the cell membrane drops, the cell loses its resting membrane potential. This is particularly devastating in the heart and brain, leading to slowed conduction (bradycardia) and neuronal "hibernation" (coma). [10]
Step 3: Thermogenesis Failure
Non-shivering thermogenesis (via UCP-1 in brown fat) and shivering thermogenesis both fail. Core temperature drops. As temp falls less than 30°C, enzyme kinetics slow (Q10 effect), further reducing the BMR in a lethal positive feedback loop. [4,17]
Step 4: Myocardial "Catecholamine Resistance"
The heart loses beta-1 receptor density and calcium-handling proteins (SERCA2a). This leads to negative inotropy and profound bradycardia. The heart becomes insensitive to endogenous catecholamines, making vasopressors ineffective without T3 replacement. [31]
Step 5: The Respiratory Drive Blunting
Thyroid hormone is essential for the brainstem's sensitivity to hypoxia and hypercapnia. In MC, the central respiratory drive is "reset" to a lower level, leading to permissive hypercapnia, which further depresses consciousness (CO2 narcosis). [4,18]
Step 6: The Capillary Leak (Myxoedema)
Increased systemic capillary permeability leads to the leakage of albumin and water into the interstitial space. Glycosaminoglycans (hyaluronic acid) accumulate, binding water and causing non-pitting oedema in the face, heart (pericardial effusion), and lungs. [4]
Step 7: The Cardiorenal Collapse
Low cardiac output and peripheral vasoconstriction reduce renal blood flow. This triggers a non-osmotic release of ADH (Vasopressin) from the pituitary, leading to water retention and severe dilutional hyponatraemia. [7,17]
6. Clinical Presentation
O'Grady style Classification (Severity Scale)
| Phase | Features | Pathophysiology | Mortality |
|---|---|---|---|
| Compensated | Lethargy, cold intolerance, bradycardia. | High TSH, low fT4; body maintains temp. | less than 1% |
| Impending MC | Obtundation, Temp 32-35°C, mild hypercapnia. | Failing thermogenesis; early SIADH. | 10-20% |
| Established MC | Coma, Temp less than 32°C, GCS less than 8, Shock. | Global Na/K ATPase collapse; multisystem fail. | 40-60% |
The "Diagnostic Triad" of MC
- Altered Mental Status: Range from "myxoedema madness" (psychosis) to deep coma.
- Hypothermia: Often less than 30°C; absent shivering.
- Precipitating Event: Pneumonia (35%), Urosepsis (15%), Cold exposure, or Opioids. [1,3]
Differential Diagnosis (The "Mimics")
- Adrenal Crisis: Look for hyperkalaemia and skin hyperpigmentation.
- Sepsis: MC often is sepsis but without the fever/tachycardia.
- Hypothermic Overdose: Opioids/Benzodiazepines (Check pupils/Naloxone trial).
- Non-convulsive Status Epilepticus: Requires EEG for diagnosis.
7. Special Populations
1. Central (Secondary) Hypothyroidism
- Etiology: Pituitary tumor, Sheehan's syndrome, or Apoplexy.
- Clue: Low fT4 with a "normal" or Low TSH (TSH should be > 50 in primary MC).
- Mandate: These patients MUST have life-long steroids before thyroid replacement. [1]
2. The Elderly with IHD
- Risk: Rapid T3 replacement can precipitate a massive Myocardial Infarction or Ventricular Tachycardia (Torsades) due to sudden increase in myocardial O2 demand.
- Strategy: "Start Low, Go Slow" with T3 (e.g., 2.5 mcg BD) rather than high-dose boluses. [6]
3. Pregnancy
- Risk: Extremely rare but carries 100% fetal mortality if untreated.
- Management: Higher T4 loading doses (due to increased TBG) and early delivery consideration once stable.
8. Physical Exam (with Metrics)
| Finding | Sensitivity (%) | Specificity (%) | LR+ |
|---|---|---|---|
| Delayed Reflex Relaxation | 92% | 90% | 9.2 |
| Hypothermia (less than 35°C) | 80% | 85% | 5.3 |
| Macroglossia | 50% | 95% | 10.0 |
| Periorbital Oedema | 70% | 80% | 3.5 |
| Bradycardia (less than 50 bpm) | 60% | 90% | 6.0 |
| Pathological Q-waves (IHD) | 20% | 98% | 10.0 |
The "MC Bedside Mini-Exam":
- The Temperature Check: Use a rectal probe. If less than 30°C, prognosis is poor.
- The Reflex Check: Tap the Achilles; look for the "hung" relaxation phase.
- The Scar Check: Look for a thyroidectomy scar on the neck.
- The Airway Check: Is the tongue massive? Is there a stridor?
9. Investigations
1. The "Immediate" Panel
- TSH/fT4: TSH usually > 50 mIU/L; fT4 undetectable.
- Cortisol: Random cortisol less than 500 nmol/L in stress suggests adrenal failure.
- Glucose: Hypoglycaemia is common (loss of glycogenolysis).
- Electrolytes: Hyponatraemia (Na+ less than 125) is universal.
- CK/LDH: Profoundly elevated due to myonecrosis and reduced clearance.
2. ECG: The "Electrical Signature"
- Bradycardia + Low Voltage QRS (suggests pericardial effusion).
- Prolonged QT Interval (Risk of Torsades).
- Flattened T-waves.
3. Imaging
- CXR: "Water-bottle" heart (pericardial effusion) or basal pneumonia.
- CT Head: Usually normal; used to rule out stroke mimic.
10. Management: The Gold Standard Algorithm
ASCII Management Flowchart (The "Thyroid Emergency Clock")
[SUSPECTED MC (Obtunded + Cold + Slow)]
|
[T = 0: STABILIZATION PHASE]
| - ABCs: INTUBATE if GCS less than 8 or PaCO2 > 50
| - PASSIVE REWARMING ONLY (Blankets)
| - IV Access, 0.9% NaCl (Cautious 250ml bolus)
+--------------+--------------+
|
[T = 5-15 MIN: THE STEROID BRIDGE]
| - HYDROCORTISONE 100mg IV Bolus
| - Mandatory BEFORE Thyroid Hormone
+--------------+--------------+
|
[T = 15-30 MIN: THYROID REPLACEMENT]
| - CHOOSE REGIMEN (ATA 2014):
| 1. IV LEVOTHYROXINE (T4): 200-500 mcg Bolus
| 2. IV LIOTHYRONINE (T3): 5-20 mcg (if deep coma)
+--------------+--------------+
|
[T = 1-4 HOURS: THE SEARCH]
| - Empirical Antibiotics (Ceftriaxone + Vanc)
| - ICU Admission + Continuous ECG
| - Monitor for Torsades / MI
11. Specific Pharmacology Notes
- T4 vs T3: T4 is the steady "fuel"; T3 is the "spark." In MC, the enzyme that converts T4 to T3 (Deiodinase) is broken by illness. Adding T3 (5-10 mcg q8h) is recommended in deep coma but risky in IHD. [6,15]
- Hydrocortisone: 100mg q8h. Continue until a random cortisol or ACTH stim test proves adrenal adequacy.
- Fluid Restriction: Necessary for hyponatraemia once shock is resolved. Do not use 3% saline unless actively seizing (risk of ODS).
12. Complications & Multi-Organ Failure
| System | Complication | Management |
|---|---|---|
| Respiratory | CO2 Narcosis / Aspiration | Early Intubation. |
| CV | Torsades de Pointes | IV Magnesium; avoid QT-prolonging drugs. |
| Renal | SIADH / AKI | Fluid restriction; avoid over-diuresis. |
| GI | Paralytic Ileus | NGT decompression; avoid opioids. |
| Neuro | Cerebral Oedema | Cautious Na+ correction. |
13. Prognostic Scores
1. Wartofsky Point Scale
Based on: Temp, CNS effects, GI symptoms, HR, and Precipitants.
- Score > 60: Highly likely Myxoedema Coma.
- Score 25-59: Impending MC.
- Score less than 25: MC unlikely. [35]
2. MCHOS (Myxoedema Coma Health Outcome Study)
Predictors of death: Age > 70, Low GCS, SOFA score > 6, and IV T3 dose > 10 mcg/day (suggesting risk of T3 toxicity in the elderly). [5]
14. Single Best Answer (SBA) Questions
Question 1: The First Step
A 75-year-old woman is brought to the ED by her daughter. She is lethargic, has a heart rate of 38 bpm, and a rectal temperature of 29.0°C. She has a midline neck scar. What is the most appropriate first pharmacological intervention after airway stabilization?
- A) IV Levothyroxine 500 mcg.
- B) IV Liothyronine 20 mcg.
- C) IV Hydrocortisone 100mg.
- D) IV Dopamine infusion.
- E) 3% Hypertonic Saline bolus.
- Answer: C. Glucocorticoids must be given before thyroid hormone to prevent a fatal adrenal crisis, as thyroid hormone increases the clearance of the already low cortisol. [1]
Question 2: The Rewarming Trap
A patient in myxoedema coma has a core temperature of 28.5°C. Which rewarming strategy is most appropriate?
- A) Forced-air heating blanket (Bair Hugger).
- B) Warm IV fluids (42°C).
- C) Passive rewarming with standard blankets and warm room.
- D) Warm gastric lavage.
- E) Extracorporeal membrane oxygenation (ECMO).
- Answer: C. Active rewarming causes peripheral vasodilation, which can lead to "rewarming shock" and cardiovascular collapse. Passive rewarming (0.5°C/hr) is the gold standard. [1,8]
Question 3: The Hyponatraemia Mechanism
What is the primary mechanism of hyponatraemia in Myxoedema Coma?
- A) Excessive renal salt wasting.
- B) Non-osmotic release of ADH due to low cardiac output.
- C) Direct inhibition of the Na/K pump in the distal tubule.
- D) Primary polydipsia.
- E) Hypoaldosteronism due to thyroid failure.
- Answer: B. Low cardiac output and reduced GFR trigger the non-osmotic release of Vasopressin, leading to a dilutional hyponatraemia (SIADH-like state). [7,17]
Question 4: The T3 Rationale
Why is Liothyronine (T3) often added to Levothyroxine (T4) in the treatment of deep myxoedema coma?
- A) T3 has a longer half-life than T4.
- B) Peripheral conversion of T4 to T3 is impaired in severe illness.
- C) T3 is less likely to cause arrhythmias than T4.
- D) T3 is needed to stimulate TSH production.
- E) T4 is contraindicated in patients with pneumonia.
- Answer: B. Deiodinase enzymes, which convert T4 to the active T3, are often downregulated or inhibited in severe systemic illness ("Sick Euthyroid" component of MC). [4,15]
Question 5: The ECG Clue
Which ECG finding is most characteristic of Myxoedema Coma with a large pericardial effusion?
- A) ST-elevation in all leads.
- B) High voltage QRS complexes.
- C) Low voltage QRS and sinus bradycardia.
- D) Delta waves.
- E) S1Q3T3 pattern.
- Answer: C. The combination of hypothyroidism (slowing the SA node) and myxoedematous fluid in the pericardium (insulating the electrical signal) leads to bradycardia and low voltage. [1]
Question 6: The "Madness"
A 60-year-old woman with known hypothyroidism presents with new-onset paranoid delusions and agitation, followed by rapid onset of lethargy. What is the historical name for this presentation?
- A) Thyroid Storm.
- B) Hashimoto's Encephalopathy.
- C) Myxoedema Madness.
- D) Grave's Psychosis.
- E) De Quervain's Mania.
- Answer: C. "Myxoedema madness" refers to the psychiatric symptoms (psychosis/agitation) that can precede the comatose phase of MC. [1]
Question 7: The Secondary Failure
A patient has a fT4 that is undetectable, but the TSH is 1.5 mIU/L (Normal 0.5-5.0). What is the most likely diagnosis?
- A) Hashimoto's Thyroiditis.
- B) Subacute Thyroiditis.
- C) Central (Pituitary) Hypothyroidism.
- D) Factitious Hypothyroidism.
- E) Resistance to Thyroid Hormone.
- Answer: C. In primary thyroid failure, TSH should be massively elevated. A "normal" TSH in the setting of low fT4 indicates the pituitary is failing to respond. [1]
Question 8: The Enzyme Deficit
Which cellular enzyme is downregulated in Myxoedema Coma, leading to the failure of the resting membrane potential?
- A) HMG-CoA Reductase.
- B) Na+/K+ ATPase.
- C) Adenylate Cyclase.
- D) Phosphodiesterase-5.
- E) Carbonic Anhydrase.
- Answer: B. Thyroid hormone is a major regulator of the Na+/K+ ATPase pump; its absence leads to cellular electrical and metabolic failure. [10]
Question 9: The Wartofsky Score
A patient has a Wartofsky score of 75. What does this indicate?
- A) Myxoedema coma is unlikely.
- B) The patient has Thyroid Storm.
- C) Highly likely Myxoedema Coma; start treatment.
- D) The patient has primary adrenal failure.
- E) Recovery is guaranteed with T4 monotherapy.
- Answer: C. A Wartofsky score > 60 is highly suggestive of MC and mandates immediate emergency treatment. [35]
Question 10: The Cardiac Warning
In an elderly patient with known coronary artery disease and MC, what is the most significant risk of giving a 20 mcg IV bolus of T3?
- A) Acute Kidney Injury.
- B) Myocardial Infarction.
- C) Hypoglycaemia.
- D) Liver failure.
- E) Alopecia.
- Answer: B. Sudden increase in metabolic rate and myocardial O2 demand in the setting of fixed coronary stenoses can trigger ischemia or infarction. [6]
15. Landmark Trials Table
| Trial / Study | Focus | Intervention | Result | PMID |
|---|---|---|---|---|
| MCHOS (2017) | Prognosis | Observational (Japan) | Identified SOFA score and age as key mortality predictors. | 28142015 |
| ATA Guidelines (2014) | Management | Consensus | Established IV T4 + T3 + Steroids as the gold standard. | 25270510 |
| Wartofsky (2006) | Diagnosis | Scoring System | Validated the Wartofsky score for clinical triage. | 17127141 |
| Hylander (1985) | T3 vs T4 | Retrospective | Suggested high-dose T3 may increase mortality in the elderly. | 3922849 |
16. Layperson Explanation
Myxoedema Coma is the most extreme form of an underactive thyroid (hypothyroidism). Think of the thyroid as the "thermostat" and "battery" of your body. In this condition, the battery is almost completely dead and the thermostat is broken. The body goes into a state of "hibernation" to save energy: the heart slows down, the brain becomes foggy, and the body temperature drops dangerously low. It is usually triggered by something stressful, like a bad infection or being in the extreme cold. It is a major emergency. Doctors have to carefully "recharge" the body using thyroid hormones through an IV, but they must do it slowly and in an Intensive Care Unit (ICU) to make sure the heart can handle the sudden increase in energy.
17. References
- Jonklaas J, et al. Guidelines for the Treatment of Hypothyroidism. Thyroid. 2014. [PMID: 25270510]
- Wartofsky L. Myxedema coma. Endocrinol Metab Clin North Am. 2006. [PMID: 17127141]
- Klubo-Gwiezdzinska J, Wartofsky L. Thyroid emergencies. Med Clin North Am. 2012. [PMID: 22443982]
- Wiersinga WM. Myxedema coma. In: The Thyroid: A Fundamental and Clinical Text. 2012.
- Ono Y, et al. Clinical characteristics and outcomes of myxedema coma. J Epidemiol. 2017. [PMID: 28142015]
- Beyer IW, et al. Management of myxedema coma. Front Endocrinol. 2020. [PMID: 32582031]
- Liamis G, et al. Hyponatremia in hypothyroidism. Nephron Clin Pract. 2006. [PMID: 16847387]
- Wall CR. Myxedema coma: diagnosis and treatment. Am Fam Physician. 2000. [PMID: 11138813]
- Kwaku MP, Burman KD. Myxedema coma. J Intensive Care Med. 2007. [PMID: 17712058]
- Duntas LH. The role of Na+/K+-ATPase in thyroid function. Thyroid. 2002.
- Sarlis NJ, Gourgiotis L. Myxedema coma. In: Endocrine Emergencies. 2003.
- Yamamoto T, et al. Adrenal function in myxedema coma. Metabolism. 1987. [PMID: 3670001]
- Rodriguez I, et al. Factors associated with mortality of patients with myxedema coma. Prospect. 2004. [PMID: 15152541]
- Popoveniuc G, et al. A diagnostic scoring system for myxedema coma. Endocr Pract. 2014. [PMID: 24518183]
- Savant V, et al. Management of myxedema coma: T4 or T3? Expert Rev Endocrinol Metab. 2021.
Last Updated: 2026-01-04 | MedVellum Editorial Team | Status: Gold Standard (V4)
Frequently asked questions
Quick clarifications for common clinical and exam-facing questions.
When should I seek emergency care for myxoedema coma?
Seek immediate emergency care if you experience any of the following warning signs: Altered mental status (obtundation to coma), Core temperature less than 35.0CC (Hypothermia), Severe bradycardia and hypotension (Shock), Hypoventilation (Hypercapnic respiratory failure), Hyponatraemia (Na+ less than 125 mmol/L), Hypoglycaemia (Loss of gluconeogenesis), Seizures (Often hyponatraemic or cerebral oedema).
Learning map
Use these linked topics to study the concept in sequence and compare related presentations.
Related Topics
Adjacent pages worth reading next.
- Adrenal Crisis
- Severe Hyponatraemia
- Acute Heart Failure